22 February 2022: Original Paper
Patient-Related Preoperative Clinical Factors Influencing 1-Year Survival After Orthotopic Heart Transplantation – A Single Center Polish Experience
Agnieszka KuczajDOI: 10.12659/AOT.934185
Ann Transplant 2022; 27:e934185
Abstract
BACKGROUND: End-stage heart failure is a growing problem in Poland. Orthotopic heart transplantation remains the best treatment option. Although increasing, the number of heart transplants is disproportionately low compared with patient need. Therefore, it is crucial to identify factors contributing to improvement of heart transplantation outcomes. To find factors providing best survival and optimal recipient selection, we analyzed pretransplant patient-related clinical factors.
MATERIAL AND METHODS: Between May 2015 and May 2020, we performed 258 cardiac transplants at our institution. We reviewed possible patient-related clinical factors affecting the 1-year survival of our patients and analyzed factors related to survival. Mean age at transplant was 53.5 (±11.8) years; 22.9% of patients were women. Preoperative factors were analyzed using univariable and multivariable analyses.
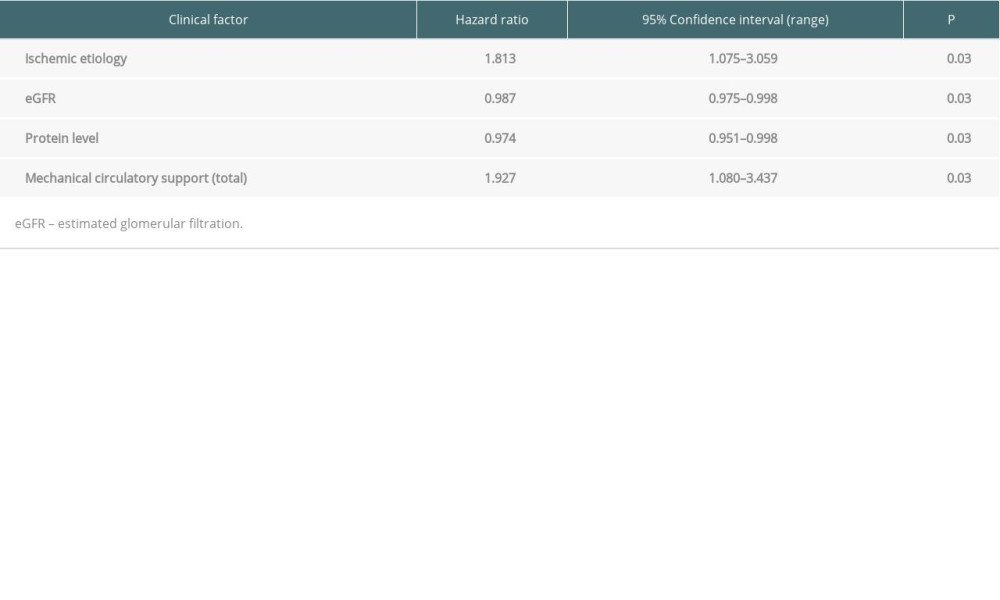
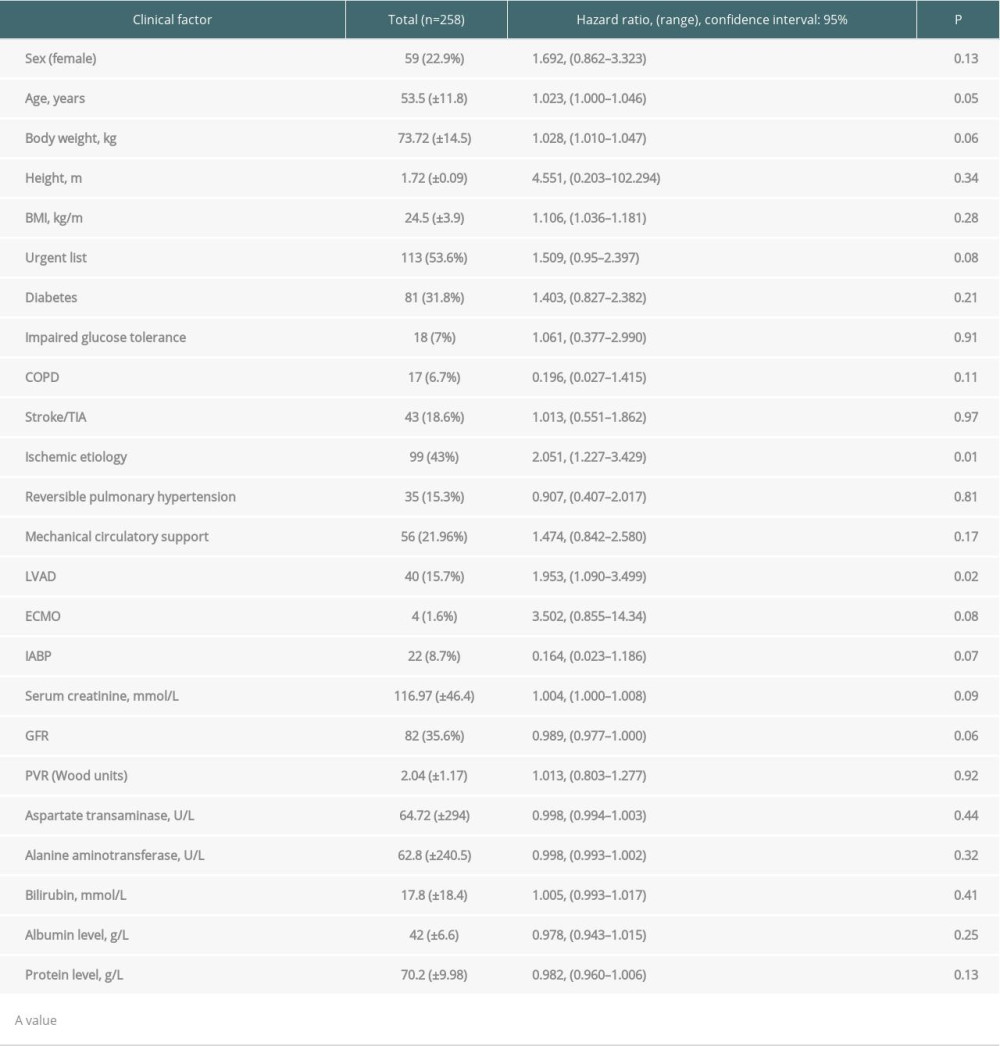
RESULTS: In this cohort, 31.8% were diabetic, 43% had ischemic etiology of heart failure, and 15.3% had reversible pulmonary hypertension. Mechanical circulatory support was used in 22%. During 1-year observation, 64 (24.8%) patients died. Univariable analysis showed ischemic etiology (hazard ratio [HR]=2.05, CI=1.227-3.429; P=0.01) and left ventricular assist device were associated with 1-year risk of death (HR=1.953, CI=1.090-3.499; P=0.02). Urgent listing trended toward worsened prognosis (HR=1.509, CI=0.95-2.397; P=0.08). Multivariable analysis showed ischemic etiology (HR=1.81, CI=1.075-3.059; P=0.03), total mechanical circulatory support (HR=1.93, CI=1.080-3.437; P=0.03), decreased eGFR (HR=0.987, CI=0.975-0.998; P=0.03), and protein level (HR=0.97, CI=0.951-0.998; P=0.04) were independently associated with worse 1-year survival after transplantation.
CONCLUSIONS: Ischemic etiology and mechanical circulatory support were the most important preoperative factors. Malnutrition and renal failure were additional risk factors. Age alone did not influence 1-year survival.
Keywords: Comorbidity, Heart Transplantation, Female, Heart-Assist Devices, Humans, Poland, Risk Factors
Background
Heart failure in developed countries is still an ongoing pandemic. According to the current guidelines, orthotopic heart transplantation (OHT) is the treatment of choice in end-stage heart failure that is refractory to medical therapy [1]. However, this procedure is performed relatively rarely in comparison to the real needs of patients. According to the current data from the Polish Transplant Coordinating Center (Poltransplant) [2], 145 patients with end-stage heart failure were transplanted in 2019, whereas at the same time, 462 patients were listed for transplantation.
To assist in the development of a system to improve the use of scarce donor resources, we attempted to identify the major preoperative factors that might identify heart transplant recipients who would were most likely to survive the first year after transplantation in our institution. As this group has not been well studied, we felt that previously published data based on larger registries may not be representative of the Polish population. Another important issue is related to the discussion between the transplant team and a potential recipient when transplantation-related risk is unacceptably high and postoperative survival is poor.
Given that mortality is highest within the first year after transplantation, we tried to find the most significant pretransplant clinical factors influencing 1-year survival. There are some data related to different patient populations. However, they cannot be fully compared with those related to the Polish population.
To optimize the risk-benefit ratio in transplant recipients, we performed a clinical analysis of heart transplant recipients to assess recipient-related factors influencing 1-year survival after OHT.
Material and Methods
STATISTICAL ANALYSIS:
Categorical variables are presented as counts and percentages. Continuous variables are presented as the mean and standard deviation for normally distributed data or the median with lower and upper quartile. The Shapiro-Wilk test was used to verify the normal distribution of data. The chi-squared test was used to compare categorical variables, whereas the
Results
During the 1-year observation period, 64 (24.8%) patients died. In the univariable analysis, ischemic etiology (
The multivariable analysis showed that ischemic etiology (HR=1.813, CI=1.075–3.059;
Univariable analysis demonstrated a nonsignificant
Discussion
Many factors, such as donor heart ischemic time, perioperative conditions (prolonged bleeding, need for high inotropic support, delayed return of graft function), and donor status, influence patient and graft survival after transplantation [3]. At the time of patients’ listing, these factors are unpredictable or can be only partially modified. On the other hand, recipient listing is a multi-stage, complex process requiring a detailed interdisciplinary approach and decision making, and we claim that some factors available at this stage may determine the course after OHT.
To find patients with the best survival after OHT, we analyzed the recipient population from a single transplant center for 5 years. We tried to concentrate on recipient clinical factors that most affected 1-year survival and could influence the decisions of transplant teams regarding the choice of the most optimal treatment for a particular patient.
A large amount of clinical data is available from the International Thoracic Organ Transplant (TTX) Registry [4]. However, the recipient population from different transplantation centers worldwide may not be fully comparable to our recipient population. Our center, similar to other Polish heart transplant centers, did not participate in the TTX Registry, and therefore the TTX Registry may have different findings. For example, in our population, the mean age at transplant was 53.5 (±11.8) years, whereas in Leiden [5], the mean age was 49 (±14) years; the difference may not be significant but shows a trend toward younger recipients. Furthermore, in the Brazilian population, the cause of transplantation was related to Chagas disease in 17.2% of patients [6], in contrast to our population, which had no cases of Chagas disease. Differences are also related to donors, organ procurement, immunosuppression, and periprocedural strategies [7].
When compared with the International Society for Heart and Lung Transplantation (ISHLT) population between 2010 and 2018, our cohort included slightly older recipients (median age 56.5 vs 55 years in the ISHLT registry), ischemic etiology was more often the indication for transplantation (43% vs 32%), and diabetes was a more prevalent comorbidity in our population (31.8%), whereas it was diagnosed in the European population in only 13.6% of cases according to the ISHLT registry [8]. However, aside from diabetes, these differences may not be statistically significant.
However, compared with that of the ISHLT registry, the 1-year mortality in our study seems to be surprisingly high. Part of the explanation may be that the statistical data available in this large registry comprise different populations, mostly outside of Europe. When compared with a German or Hispanic population, which are also included in this registry, the current 1-year mortality rate is rather similar, equally around 20% [9,10].
Based on the multivariable model, in our population, we showed adverse effects of decreased eGFR calculated by the Modification of Diet in Renal Disease Study equation on 1-year survival. This finding is comparable to the observations of other studies [11–13]. Similarly, in the present study, we found that patients with ischemic etiology of heart failure had less favorable survival, which is in line with the results of other studies. Coronary artery disease is a part of the generalized atherosclerotic processes, and patients with coronary artery disease are more prone to vascular complications, such as ischemic stroke.
Of note, neither diabetes nor age at the time of transplant was correlated with survival in our group of patients. However, we suppose that the influence of these factors could reach statistical significance in the long-term follow-up. A similar observation was made in terms of pulmonary vascular resistance in our patients. According to the current guidelines [14], we did not perform transplants in patients with irreversible pulmonary hypertension. However, patients with reversible pulmonary hypertension type 2 were given sildenafil orally if it was not contraindicated. It may also be a result of appropriate patient selection (the sodium nitroprusside vasoreactivity test was performed in the whole group of patients as the part of qualification) and adherence to the ISHLT guidelines.
The ISHLT registry showed some differences between patients with higher and lower body mass indexes (BMI). In our study, univariable or multivariable analyses showed no influence of BMI on survival, which may have been related to the relatively small number of patients.
We observed that poor nutritional status, defined by protein concentration and not by BMI, was a factor for a poorer prognosis. In our cohort of patients, a higher protein level, but not albumin, was correlated with better survival. We think that frequent supplementation of an intravenous albumin preparation in cases of hypoalbuminemia may disturb this correlation that is observed in available studies [15]. A low protein level in patients is associated with poorer postoperative wound healing, poor rehabilitation, and decreased immune defense against infections [14]. Therefore, it seems reasonable to try to improve patient nutritional status before transplantation.
Worsened survival of OHT patients after previous left ventricular assist device implantation should be interpreted with caution. The long-term observation of patients with a left ventricular assist device is ongoing, and it cannot be excluded that transplantation might be the best long-term option for this group of patients, despite an elevated risk of complications as compared with that in other transplant patients.
Furthermore, in univariable analysis, mechanical circulatory support (in total) did not influence survival, whereas in multivariable analysis, the relationship reached statistical significance. In univariable analysis, particular types of mechanical circulatory support influenced survival in opposite directions (IABP improved survival), which may suggest that the whole group of circulatory support is inhomogeneous and the group of short-term circulatory support has a different clinical profile from the long-term group. Multivariable analysis considering the differences between these 2 groups showed less favorable outcomes in the group with mechanical circulatory support. This is in line with speculations, as this group of patients is the most seriously ill subgroup of patients awaiting transplantation.
Studies have shown that the 2-year survival after left ventricular assist device support was as good as after OHT, which suggests that destination therapy may be a better option than subsequent OHT in some patients with multimorbidity (limiting survival) after long-term mechanical circulatory support implantation [16].
In some cases, the risk-benefit ratio may be unacceptably high, and conservative treatment would be the best option for some patients and those listed for transplantation with a more favorable clinical profile. If the decision to transplant is made, the patient and the transplant team should be aware of the high risk of adverse events.
Further directions may be implementing nutritional programs in patients with advanced heart failure listed for heart transplantation. Notable is also the visible discrepancy in number and percentage of transplanted women and men. Also, the overt difference between 1-year mortality in European countries and the whole TTx registry needs further explanation.
Conclusions
Ischemic etiology and preoperative demand for mechanical circulatory support were the most important preoperative factors worsening 1-year survival rates in heart transplant recipients in the single-center Polish population. Malnutrition and renal failure were additional risk factors. Age alone did not influence 1-year survival. Our results show differences between the ISHLT registry population and our cohort. Data and conclusions from large registries covering different populations should be interpreted with caution. Long-term studies are needed to show the potential benefit of long-term mechanical circulatory support over subsequent transplantation in multimorbid patients.
We did not analyze death cases because they were influenced by many factors. Due to the relatively small number of patients, the analysis of particular death cases and endpoints were not performed. We also did not concentrate on perioperative and donor-related risk factors because they are unpredictable at the time of patients’ listing. A multicenter analysis of Polish recipients could more accurately answer some of these questions.
References
1. Ponikowski P, Voors AA, Anker SD, 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: Eur Heart J, 2016; 37; 2129-200
2. Malanowski P, Grzywacz A, Łęczycka A, Poltransplant: Biuletyn Informacyjny 2020, 2020; 1(29) [in Polish]
3. Schulze PCh, Jiang J, Yang J, Preoperative assessment of high-risk candidates to predict survival after heart transplantation: Circ Heart Fail, 2013; 6; 527-34
4. : Registry Data Slides Available from: [cited 2021 Sept 10]https://ishlt.org/research-data/registries/ttx-registry/ttx-registry-slides
5. Van Cleemput JJA, Verbelen TOM, Van Aelst LML, How to obtain and maintain favorable results after heart transplantation: keys to success?: Ann Cardiothorac Surg, 2018; 7(1); 106-17
6. Custódio IL, Lima FET, Lopes MVO, Results of medium-term survival in patients undergoing cardiac transplantation: Institutional experience: Rev Bras Cir Cardiovasc, 2013; 28(4); 470-76
7. Kim IC, Youn JC, Kobashigawa JA, The past, present and future of heart transplantation: Korean Circ J, 2018; 48(7); 565-90
8. , Heart Transplantation: Adult recipients, 2019 [cited on]. Available from:https://ishltregistries.org/registries/slides.asp?yearToDisplay=2019
9. Gummert JF, Heart transplantation in Bad Oeynhausen, Germany: The Heart Transplant program at the Heart and Diabetes Center Bad Oeynhausen, University Hospital, Ruhr – University Bochum University, Germany: Eur Heart J, 2017; 38(46); 3411-13
10. Gonzalez-Vilchez F, Almenar-Bonet L, Crespo-Leiro MG: Rev Esp Cardiol (Engl Ed), 2021; 74(11); 962-70
11. Foroutan F, Alba AC, Guyatt G, Predictors of 1-year mortality in heart transplant recipients: A systematic review and meta-analysis: Heart, 2018; 104; 151-60
12. Kuśmierczyk M, Różański J, Zembala M, Heart failure in Poland: Left ventricular assist device destination therapy and other challenges of interventional cardiology and cardiac surgery: J Cardiol, 2020; 27(6); 693-704
13. Moayedi Y, Fan CPS, Cherigh WS, Survival outcomes after heart transplantation. Does recipient sex matter?: Circ Heart Fail, 2019; 12; e006218
14. Mehra MR, Canter CE, Hanan MM, The 2016 International Society for Heart Lung Transplantation listing criteria for heart transplantation: A 10-year update (Guidelines): J Heart Lung Transplant, 2015; 25(1); 1-23
15. Kato TS, Cheema FH, Yang J, Preoperative serum albumin levels predict 1-year postoperative survival of patients undergoing heart transplantation: Circ Heart Fail, 2013; 6(4); 785-91
16. Mechanick JI, Practical aspects of nutritional support for wound-healing patients: Am J Surg, 2004; 188; 52-56
In Press
Original article
Diagnostic Utility of FAR1 Methylation Levels in Hepatocellular Carcinoma Patients Undergoing Liver Transpl...Ann Transplant In Press; DOI: 10.12659/AOT.951568
Original article
Inferior Long-Term Outcome of Fatty Liver Allografts After Orthotopic Liver TransplantationAnn Transplant In Press; DOI: 10.12659/AOT.950589
Database Analysis
Identification and Validation of Liver Transplantation-Induced Acute Lung Injury Biomarkers Using a Bioinfo...Ann Transplant In Press; DOI: 10.12659/AOT.950289
Original article
Survival and Recurrence in Liver Transplant Patients With Intrahepatic Cholangiocarcinoma and Hepatocellula...Ann Transplant In Press; DOI: 10.12659/AOT.950997
Most Viewed Current Articles
24 Aug 2021 : Review article 18,372
Normothermic Machine Perfusion (NMP) of the Liver – Current Status and Future PerspectivesDOI :10.12659/AOT.931664
Ann Transplant 2021; 26:e931664
05 Apr 2022 : Original article 14,731
Impact of Statins on Hepatocellular Carcinoma Recurrence After Living-Donor Liver TransplantationDOI :10.12659/AOT.935604
Ann Transplant 2022; 27:e935604
22 Nov 2022 : Original article 14,244
Long-Term Effects of Everolimus-Facilitated Tacrolimus Reduction in Living-Donor Liver Transplant Recipient...DOI :10.12659/AOT.937988
Ann Transplant 2022; 27:e937988
29 Dec 2021 : Original article 13,752
Efficacy and Safety of Tacrolimus-Based Maintenance Regimens in De Novo Kidney Transplant Recipients: A Sys...DOI :10.12659/AOT.933588
Ann Transplant 2021; 26:e933588