14 May 2021: Original Paper
Nationwide Survey of Post-Transplant Glomerular Diseases, Based on the Japan Renal Biopsy Registry (J-RBR)
Joichi UsuiABCDEFG, Kunihiro YamagataABCDE, Michio NagataABCDE, Akira ShimizuBDE, Asami TakedaBDE, Hitoshi SugiyamaBDE, Hiroshi SatoBDE, Hitoshi YokoyamaBDEDOI: 10.12659/AOT.931873
Ann Transplant 2021; 26:e931873
Abstract
BACKGROUND: Nationwide data on allograft kidney biopsies have been limited in number, in contrast to the large amount of accumulated data on native kidney biopsies. In this context, we have surveyed transplant biopsy data based on the nationwide database, the Japan Renal Biopsy Registry (J-RBR).
MATERIAL AND METHODS: A total of 2430 transplant biopsy cases were registered in the web-based J-RBR from January 2007 to January 2018. We categorized the entries regarding both the purpose of the biopsy and pathological diagnosis, and confirmed transplant glomerular diseases based on the clinical and pathological diagnosis.
RESULTS: Of the 2430 total transplant biopsy cases, 637 cases, including 9 cases of baseline biopsy, 216 cases of protocol biopsy, and 232 cases of episode biopsy, had a pathological diagnosis, including glomerular diseases, rejection, calcineurin inhibitor nephropathy, and interstitial fibrosis and tubular atrophy. Of these, 127 cases presented with glomerular disease, including 8 cases of baseline biopsy, 23 of protocol biopsy, 59 of episode biopsy, and 37 of unknown purpose). A total of 127 biopsies with glomerular disease revealed a high prevalence of immunoglobulin A nephropathy (n=38, 29.9%), followed by mesangial proliferative glomerulonephritis (n=29, 22.8%) and focal segmental glomerulosclerosis (n=8, 6.3%) when focused on protocol and episode biopsies.
CONCLUSIONS: The nationwide transplant biopsy database demonstrated the pathological characteristics of 637 cases, including 127 cases of post-transplant glomerular disease. The protocol and episode biopsies included high prevalence rates of IgAN, followed by FSGS.
Keywords: Glomerulonephritis, IGA, Kidney Transplantation, Pathology, Biopsy, Japan, Kidney, Registries
Background
Post-transplant glomerular disease has a strong impact on kidney allograft failure and long-term graft survival. Glomerular disease accounts for about 30% of end-stage kidney disease (ESKD), and its recurrence after transplantation leads to a decline in kidney allograft function and graft loss [1]. The post-transplant glomerular diseases identified included various characteristics, including not only recurrent glomerular disease but also transmitted glomerular disease and
Material and Methods
ENTRIES BASED ON THE J-RBR:
We analyzed transplant biopsy data from all over the country based on the J-RBR, which was launched in 2007 by the Committee for the Standardization of Renal Pathological Diagnosis and the Committee for the Kidney Disease Registry of the Japanese Society of Nephrology. It is a nationwide, web-based, and prospective registry system in Japan [2]. The registry includes patient data on the clinical diagnosis, histological diagnosis based on the pathogenesis, and histological diagnosis based on a histopathological examination with additional information. The pathological diagnosis was made by nephrologists, nephropathologists, and pathologists, depending on each institution. The J-RBR appears in the Clinical Trial Registry of UMIN (registration number UMIN 000000618), and the Ethics Review Board of the Japanese Society of Nephrology and each research institution approved the study in accordance with the Declaration of Helsinki (The University of Tsukuba Hospital, No. H20-330). Written informed consent was obtained from all the patients who participated in the J-RBR. In the present sub-study, we surveyed all entries from January 2007 to January 2018 and selected cases with kidney allograft biopsy. The present sub-study was approved by the Ethics Review Board of the University of Tsukuba Hospital (No. H30-253).
THE DIAGNOSTIC CLASSIFICATION OF THE J-RBR:
In the J-RBR, clinical diagnoses were divided into these categories: acute nephritic syndrome, rapidly progressive nephritic syndrome, recurrent or persistent hematuria, chronic nephritic syndrome, nephrotic syndrome, renal disorder with metabolic disorder, renal disorder with collagen disease or vasculitis, hypertensive nephropathy, inherited renal disease, acute renal failure, drug-induced nephropathy, renal transplantation, congenital renal urinary tract abnormalities, polycystic kidney disease, hemolytic uremic syndrome/thrombotic thrombocytopenic purpura, and others. Next, the histological diagnoses based on the pathogenesis were classified into categories, including primary glomerular disease except IgAN, IgAN, purpura nephritis, lupus nephritis, Myeloperoxidase (MPO)-anti-neutrophil cytoplasmic antibody (ANCA)-positive nephritis, Proteinase 3 (PR3)-ANCA-positive nephritis, anti-glomerular basement membrane antibody nephritis, hypertensive nephrosclerosis, thrombotic microangiopathy, diabetic nephropathy (DN), amyloid nephropathy, Alport syndrome, thin basement membrane disease, infection-related nephropathy, transplanted kidney, and others. Finally, histological diagnoses based on a histopathological examination were divided into these categories: minor glomerular abnormalities, FSGS, membranous glomerulonephritis (MGN), mesangial proliferative glomerulonephritis (MesPGN), endocapillary proliferative glomerulonephritis, MPGN types I and III, dense deposit disease, crescentic and necrotizing glomerulonephritis, sclerosing glomerulonephritis, nephrosclerosis, acute interstitial nephritis, chronic interstitial nephritis, acute tubular necrosis, transplanted kidney, and others.
CLINICOPATHOLOGICAL PARAMETERS AND STATISTICS:
Other than the clinical diagnosis, histological diagnosis based on the pathogenesis, and histological diagnosis based on histopathological examination, each patient’s data contained additional information, including the timing and reason for the biopsy and the pathological findings. Information on the timing and reason for the transplant biopsy was divided into baseline, protocol, and episode, on the basis of additional comments in questionnaires from each institution. Baseline biopsies included both time-zero and 1-hour post-reperfusion biopsies. The timing of the protocol biopsies varied depending on the institution. Episode biopsies included cases such as elevation of serum creatinine, proteinuria and hematuria. Cases without any information on the timing of the transplantation were categorized as unknown. As for pathological findings, we focused on 4 categories, namely glomerular diseases, rejection, calcineurin inhibitor (CNI) nephropathy, and interstitial fibrosis and tubular atrophy (IF/TA), as representative. Duplicates were allowed in these pathological findings. Data on age and creatinine are presented as means ± standard deviation.
Results
DIAGNOSIS AND CLASSIFICATION IN ALL 2430 CASES:
A total of 2430 cases, categorized as “transplanted kidney” cases in the histological diagnosis based on the pathogenesis, were selected for this investigation on kidney allograft biopsy. As for the clinical diagnoses, 2379 cases were categorized as renal transplantations, 4 cases as acute nephritic syndrome, 3 cases as rapidly progressive nephritic syndrome, 36 as chronic nephritic syndrome (of these 36 cases, 23 cases were also labeled as renal transplantation), 5 cases as nephrotic syndrome, 1 case as renal disorder with metabolic disorder, 2 cases as hypertensive nephropathy, 1 case as inherited renal disease, 1 case as acute renal failure, 1 case as drug-induced nephropathy, 11 cases as congenital renal urinary tract abnormalities, and 9 cases as others.
As for the histological diagnoses based on a histopathological examination, 2356 cases were transplanted kidney cases, followed by 8 cases of minor glomerular abnormalities, 1 of FSGS, 2 of MGN, 3 of MesPGN, 1 of endocapillary proliferative glomerulonephritis, 3 of MPGN (types I and III), 1 of dense deposit disease, 1 of crescentic and necrotizing glomerulonephritis, 1 of sclerosing glomerulonephritis, 5 of acute interstitial nephritis, 4 of chronic interstitial nephritis, 9 of acute tubular necrosis, and 35 others.
TRANSPLANT BIOPSY WITH HISTOPATHOLOGICAL FINDINGS:
Of the 2430 total transplant biopsy cases, 1793 cases were excluded from the present investigation because they were lacking a pathological diagnosis (Figure 1). The remaining 637 cases included 9 cases of baseline biopsy, 216 cases of protocol biopsy, 232 cases of episode biopsy, and 220 cases with an unknown cause for the biopsy. Of these 637 cases, post-transplant glomerular disease was diagnosed in 127 cases.
CLINICAL CHARACTERISTICS OF RENAL ALLOGRAFT BIOPSIES:
Table 1 shows the clinical characteristics of the renal allograft biopsies, including age, sex, urinary protein level, hematuria, serum creatinine, and histopathological diagnosis, represented as glomerulonephritis, rejection, CNI nephropathy, and IF/TA. In 637 cases, the age on average was 41.3±15.4, with 403 males and 234 females; 223 cases presented with proteinuria (more than 1+) and 172 cases with hematuria (more than 1+). The serum creatinine level was 2.2±1.9 mg/dL in total, 7.8±3.7 mg/dL in baseline, 1.4±0.3 mg/dL in protocol, 2.5±2.0 mg/dL in episode, and 2.3±2.0 mg/dL in unknown cause. As for the histopathological diagnoses, glomerular disease was found in 127 cases, rejection in 235 cases, CNI nephropathy in 80 cases, and IF/TA in 44 cases. Of the 127 cases of glomerular disease, 8 were in baseline, 23 in protocol, 59 in episode, and 37 in unknown cause, respectively.
POST-TRANSPLANT GLOMERULAR DISEASE:
The histopathological diagnoses in cases of biopsy-proven glomerular disease were divided into IgAN, FSGS, MGN, MPGN, MesPGN, DN, and others (Table 2). The cases were also classified into transmission, recurrence, and unknown for each type of biopsy. Even though none of the cases were clearly described as de novo glomerular disease, “unknown” cases may also include de novo glomerular diseases.
A total of 127 biopsies with glomerular disease revealed a high prevalence of IgAN (n=65, 51.2%), followed by MesPGN (n=31, 24.4%) and FSGS (n=13, 10.2%). The number of baseline biopsies was limited, but these biopsies showed a high prevalence of transmission of IgAN from donors compared to other glomerular diseases. In protocol and episode biopsies, the prevalence was the highest for IgAN, with 38 cases (29.9%), 14 in protocol biopsies and 24 in episode, followed by MesPGN, with 29 cases (22.8%), 6 in protocol and 23 in episode, and FSGS, with 8 cases (6.3%), 2 in protocol and 6 in episode.
The number of cases of IgAN recurrence was 5 in protocol and 21 in episode, accounting for the highest number compared to other glomerular diseases. In addition, MesPGN cases may include IgAN, suggesting that the number of recurrent IgAN cases may have actually been higher. Combining the cases from protocol, episode, and unknown, excluding baseline cases, the number of recurrence cases was 46 for IgAN, 6 for FSGS, 1 for MGN, 0 for MPGN, 2 for MesPGN, and 0 for DN. In addition, as described above, most of the MesPGN cases were presumed to be IgAN.
Discussion
Graft survival has improved year by year, and after 2010, the graft survival rate was 98.7% at 1 year and 94.3% at 5 years for living donor transplants and 96.7% at 1 year and 88.0% at 5 years for deceased donor transplants in Japan (
Nationwide data on post-transplant glomerular disease are limited, but 4 studies referred to its prevalence, shown in Table 3 [1,5–7]. The number of allograft kidney biopsy, the prevalence of pre- and post-transplant glomerular disease, and the recurrence rate of glomerular disease were all addressed in these studies. In the present study, there was a total of 127 cases of post-transplant glomerular disease, including 38 cases (29.9%) of IgAN and 8 cases (6.3%) of FSGS when focused on protocol and episode biopsies, excluding the baseline and unknown categories. As for the recurrence of glomerular diseases, there were 33 cases in protocol and episode biopsies, including 26 cases (78.8%) of IgAN and 4 cases (12.1%) of FSGS. In the data from countries other than Japan, either post-transplant glomerular disease or the recurrence of glomerular disease or both were given, with IgAN showing the highest number of cases followed by FSGS in most of these studies, except for a survey from the USA. These findings were similar to those of the present study.
Some risk factors have been reported for the development of recurrent glomerular diseases. For example, in recurrent IgAN, young age, male sex, a rapidly progressive course of the original disease before transplantation, the presence of specific HLA genotypes, no HLA mismatch, and high serum IgA levels have been reported to be risk factors [8–10]. For FSGS, recurrent risk factors include young age, rapid progression to ESKD, bilateral nephrectomy, White race, and loss of a previous allograft due to FSGS recurrence [11,12]. Preventive measures, represented as perioperative rituximab and therapeutic plasma exchange, have been studied, but post-transplant recurrence of FSGS remains unresolved.
In the present study, even though the total number was limited when focused on glomerular disease, the high prevalence rates of IgAN and FSGS showed the same trend as in previous studies. In addition, MesPGN in this study might include IgAN, suggesting the possibility that there were more cases of recurrent IgAN. Considering the fact that the prevalence of IgAN is higher in Eastern Asian countries than in North America or European countries, further studies from Japan may help achieve a better allograft prognosis. The present study has 3 limitations. First, the timing of the baseline and protocol biopsies were different depending on the institution. For example, the baseline biopsies included both 0-hour and 1-hour biopsies. Second, the registry form was not fully established for accumulating allograft biopsy data, resulting in there being limited information on the timing of the biopsies and the clinical course. However, the registry was renewed in 2018 and the current system is now suitable not only for native kidney biopsies but also for allograft biopsies. We are aiming to analyze these newly accumulated data with our present data in the near future. Third, the diagnostic ability varied across institutions, which caused difficulties in integrating the information. Our future task is to close diagnostic gaps among institutions and to standardize pathological diagnosis.
Conclusions
The present study is the first to show the whole picture of transplant kidney biopsy in Japan. Nationwide renal transplant data are limited even in other countries, suggesting the importance of accumulating integrated data. This registry is ongoing with more specific data on kidney transplantation, and further studies with more detailed information are needed, with the goals of tackling the recurrence of glomerular disease and attaining better graft survival.
References
1. Allen PJ, Chadban SJ, Craig JC, Recurrent glomerulonephritis after kidney transplantation: risk factors and allograft outcomes: Kidney Int, 2017; 92(2); 461-69
2. Sugiyama H, Yokoyama H, Sato H, Japan Renal Biopsy Registry: The first nationwide, web-based, and prospective registry system of renal biopsies in Japan: Clin Exp Nephrol, 2011; 15(4); 493-503
3. Hickson LJ, El-Zoghby ZM, Lorenz EC, Patient survival after kidney transplantation: Relationship to pretransplant cardiac troponin T levels: Am J Transplant, 2009; 9(6); 1354-61
4. Morozumi K, Takeda A, Otsuka Y, Recurrent glomerular disease after kidney transplantation: An update of selected areas and the impact of protocol biopsy: Nephrology (Carlton), 2014; 19(Suppl 3); 6-10
5. Hariharan S, Adams MB, Brennan DC, Recurrent and de novo glomerular disease after renal transplantation: A report from renal allograft disease registry: Transplant Proc, 1999; 31(1–2); 223-24
6. Chailimpamontree W, Dmitrienko S, Li G, Probability, predictors, and prognosis of posttransplantation glomerulonephritis: J Am Soc Nephrol, 2009; 20(4); 843-51
7. An JN, Lee JP, Oh YJ, Incidence of post-transplant glomerulonephritis and its impact on graft outcome: Kidney Res Clin Pract, 2012; 31(4); 219-26
8. Avasare RS, Rosenstiel PE, Zaky ZS, Predicting post-transplant recurrence of IgA nephropathy: The importance of crescents: Am J Nephrol, 2017; 45(2); 99-106
9. Andresdottir MB, Haasnoot GW, Persijn GG, Claas FH, HLA-B8, DR3: A new risk factor for graft failure after renal transplantation in patients with underlying immunoglobulin A nephropathy: Clin Transplant, 2009; 23(5); 660-65
10. Garnier AS, Duveau A, Demiselle J, Early post-transplant serum IgA level is associated with IgA nephropathy recurrence after kidney transplantation: PLoS One, 2018; 13(4); e0196101
11. Ponticelli C, Recurrence of focal segmental glomerular sclerosis (FSGS) after renal transplantation: Nephrol Dial Transplant, 2010; 25(1); 25-31
12. Kienzl-Wagner K, Waldegger S, Schneeberger S, Disease recurrence-the sword of damocles in kidney transplantation for primary focal segmental glomerulosclerosis: Front Immunol, 2019; 10; 1669
Figures
Tables
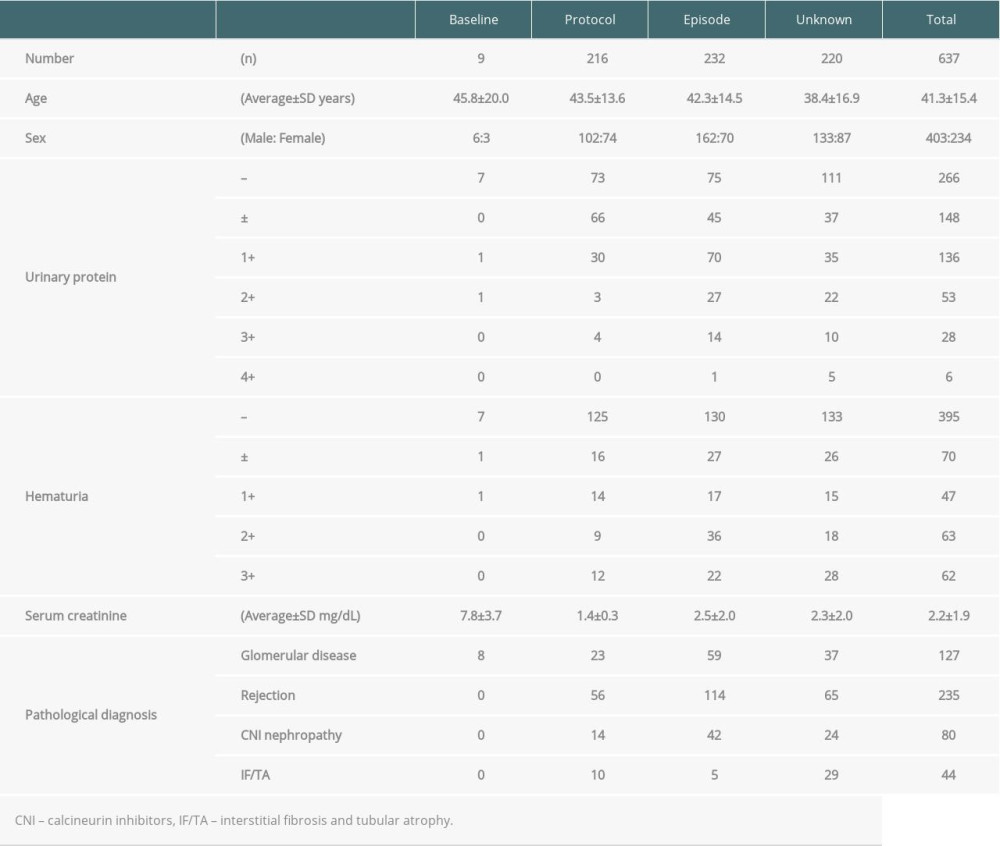 Table 1. Clinicopathological characteristics of renal allograft biopsies.
Table 1. Clinicopathological characteristics of renal allograft biopsies.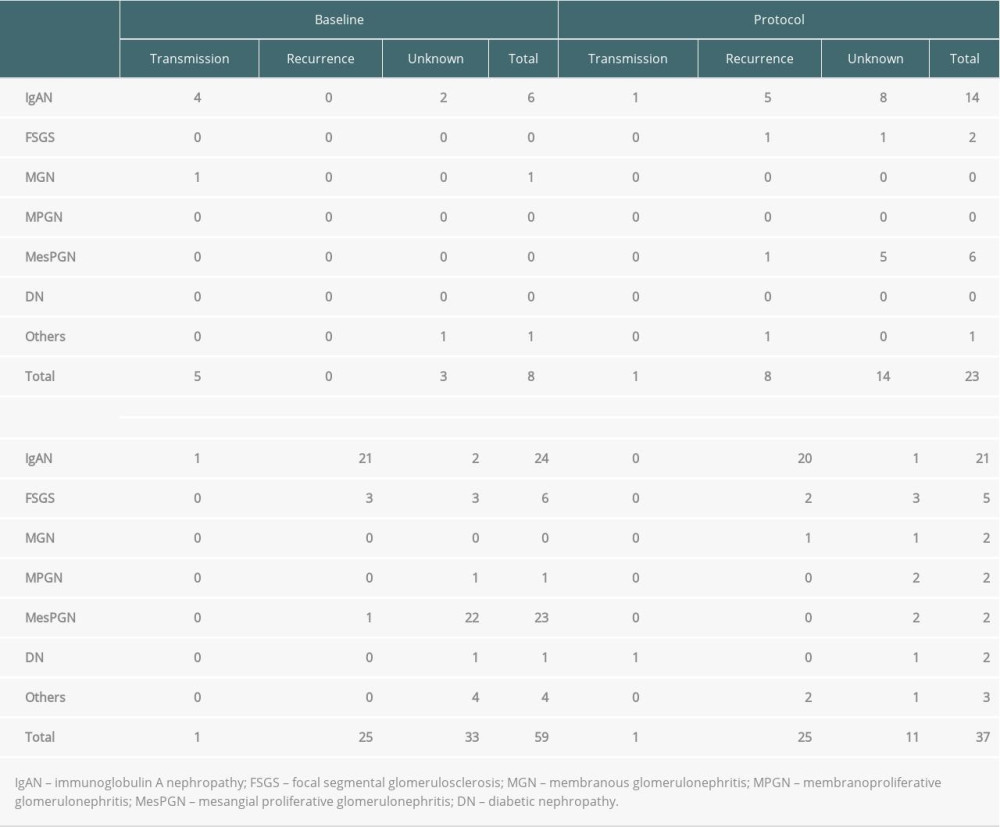 Table 2. Pathological diagnosis in biopsy-proven glomerular diseases.
Table 2. Pathological diagnosis in biopsy-proven glomerular diseases.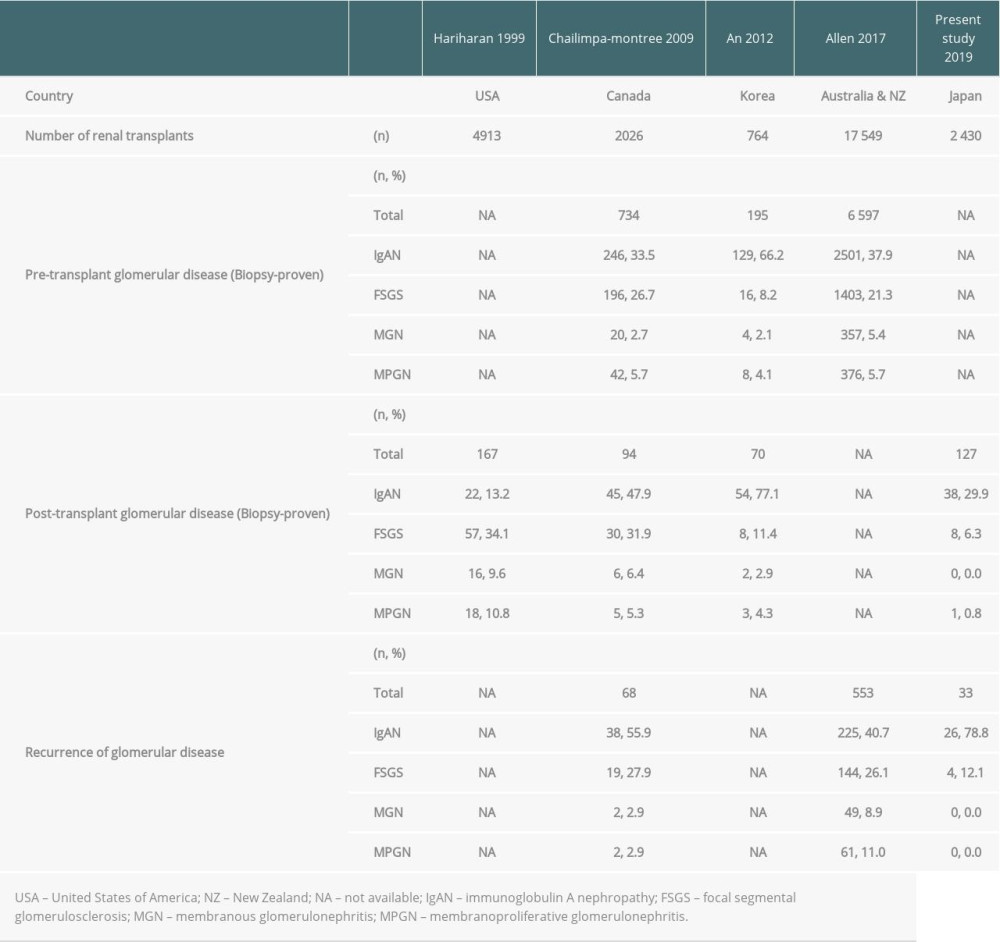 Table 3. Characteristics of post-transplant glomerular diseases obtained from nationwide survey.
Table 3. Characteristics of post-transplant glomerular diseases obtained from nationwide survey. Table 1. Clinicopathological characteristics of renal allograft biopsies.
Table 1. Clinicopathological characteristics of renal allograft biopsies. Table 2. Pathological diagnosis in biopsy-proven glomerular diseases.
Table 2. Pathological diagnosis in biopsy-proven glomerular diseases. Table 3. Characteristics of post-transplant glomerular diseases obtained from nationwide survey.
Table 3. Characteristics of post-transplant glomerular diseases obtained from nationwide survey. In Press
15 Mar 2024 : Review article
Approaches and Challenges in the Current Management of Cytomegalovirus in Transplant Recipients: Highlighti...Ann Transplant In Press; DOI: 10.12659/AOT.941185
18 Mar 2024 : Original article
Does Antibiotic Use Increase the Risk of Post-Transplantation Diabetes Mellitus? A Retrospective Study of R...Ann Transplant In Press; DOI: 10.12659/AOT.943282
20 Mar 2024 : Original article
Transplant Nephrectomy: A Comparative Study of Timing and Techniques in a Single InstitutionAnn Transplant In Press; DOI: 10.12659/AOT.942252
28 Mar 2024 : Original article
Association Between FEV₁ Decline Rate and Mortality in Long-Term Follow-Up of a 21-Patient Pilot Clinical T...Ann Transplant In Press; DOI: 10.12659/AOT.942823
Most Viewed Current Articles
05 Apr 2022 : Original article
Impact of Statins on Hepatocellular Carcinoma Recurrence After Living-Donor Liver TransplantationDOI :10.12659/AOT.935604
Ann Transplant 2022; 27:e935604
12 Jan 2022 : Original article
Risk Factors for Developing BK Virus-Associated Nephropathy: A Single-Center Retrospective Cohort Study of ...DOI :10.12659/AOT.934738
Ann Transplant 2022; 27:e934738
22 Nov 2022 : Original article
Long-Term Effects of Everolimus-Facilitated Tacrolimus Reduction in Living-Donor Liver Transplant Recipient...DOI :10.12659/AOT.937988
Ann Transplant 2022; 27:e937988
15 Mar 2022 : Case report
Combined Liver, Pancreas-Duodenum, and Kidney Transplantation for Patients with Hepatitis B Cirrhosis, Urem...DOI :10.12659/AOT.935860
Ann Transplant 2022; 27:e935860









