12 October 2021: Original Paper
Prognostic Role of Serum Albumin Level in Patients with Lymphoma Undergoing Autologous Stem Cell Transplantation
Chengxin Luo12CDE, Qingrong Li12B, Xi LiDOI: 10.12659/AOT.933365
Ann Transplant 2021; 26:e933365
Abstract
BACKGROUND: High-dose chemotherapy followed by autologous stem cell transplantation (HDT/ASCT) plays a crucial role in the therapy of patients with lymphoma. This retrospective study aimed to analyze prognostic factors in patients undergoing HDT/ASCT for lymphoma.
MATERIAL AND METHODS: We included patients with lymphoma who underwent HDT/ASCT at our center. Time-to-event outcomes, including progression-free survival (PFS) and overall survival (OS), were analyzed with the Kaplan-Meier method and log-rank test. Receiver operating characteristic (ROC) curve analysis and Cox proportional hazard regression analysis were performed to explore the prognostic value of different factors.
RESULTS: A total of 113 patients with lymphoma were included. Patients with low serum albumin levels (<37 g/L) before transplantation had significantly lower PFS and OS (P<0.01). Albumin levels before transplantation significantly predicted early progression (progressed within 1 year) after transplantation (AUC=0.706, P=0.003). Multivariate Cox analysis indicated that low albumin level (hazard ratio [HR] 3.19, 95% confidence interval [CI] 1.54-6.63; P=0.002) and age >60 years (HR 2.92, 95% CI 1.27-6.71; P=0.012) were independent risk factors for PFS. Total protein <60 g/L was an independent risk factor for OS (HR 3.57, 95% CI 1.45-8.78; P=0.006).
CONCLUSIONS: Low albumin level before transplantation was an independent risk factor in patients with lymphoma undergoing HDT/ASCT. Intense care and effective maintenance therapy after transplantation are required for patients with low albumin levels.
Keywords: Albumins, Survival, Humans, Serum Albumin, Human, Transplantation, Autologous
Background
Lymphoma is one of the most common malignancies, accounting for approximately 3% of cancer cases and cancer-related mortality worldwide [1]. Over the past 2 decades, the incorporation of novel agents into conventional chemotherapy treatment led to significant improvements in disease control and survival of patients with lymphoma [2,3]. However, the outcomes of patients who have high-risk disease and who experienced relapse after first-line therapy remain poor. High-dose chemotherapy followed by autologous stem cell transplantation (HDT/ASCT) is the standard of care for these patients. Data from randomized controlled trials have established that upfront consolidative ASCT for high-risk patients with lymphoma who have achieved complete response (CR) and salvage therapy with HDT/ASCT for patients with relapsed or refractory lymphoma could significantly prolong progression-free survival (PFS) [4–7].
Despite the durable disease control achieved with HDT/ASCT in a subset of patients with lymphoma, disease relapse remains the most common cause of death. About 30% to 50% of patients had relapse or disease progression within 3 years after ASCT, implying the requirement of post-ASCT maintenance/consolidation therapy [4–8]. Maintenance therapy with rituximab for patients with non-Hodgkin lymphoma (NHL) or brentuximab vedotin for patients with Hodgkin lymphoma (HL) could yield superior PFS compared with observation or placebo [9–11]. However, these agents are associated with a high financial burden and a series of undesired toxic effects. Therefore, it is important to precisely identify those patients who are most likely to benefit from HDT/ASCT and post-transplantation maintenance therapy.
Investigation of prognostic factors that are associated with the high risk of progression or relapse after HDT/ASCT in patients with lymphoma would be helpful for the precise application of maintenance in clinical practice. Previous studies have shown that higher serum levels of albumin at diagnosis are associated with superior survival outcomes in patients with diffuse large B-cell lymphoma (DLBCL), but the prognostic role of albumin levels before transplantation in patients with lymphoma undergoing HDT/ASCT remains unknown [12,13]. Therefore, we aimed to explore the prognostic value of albumin level and to identify other prognostic factors by conducting a retrospective study in patients with lymphoma who received HDT/ASCT at our center.
Material and Methods
PATIENT SELECTION:
This retrospective study was approved by the Ethics Committee of Southwest Hospital, Third Military Medical University (Chongqing, China, approval no. KY2020200) and was in accordance with the principles of the Declaration of Helsinki. Patients with lymphoma who received HDT/ASCT between January 2006 and August 2019 at the Center for Hematology in Southwest Hospital (Chongqing, China) were included in the study. Eligible patients for ASCT were <70 years old and had a biopsy-confirmed diagnosis of NHL or HL, adequate organ function, and an Eastern Cooperative Oncology Group performance status (ECOG PS) of 3 or less. The choice of induction therapy or salvage chemotherapy regimen prior to ASCT varied based on patient diagnosis. All transplantation procedures were performed according to standard protocol. Autologous peripheral blood stem cells were collected following mobilization using granulocyte colony-stimulating factor alone or in combination with chemotherapy. The acceptable minimal dose was 2×106 CD34+ cells/kg or 3×108 mononuclear cells/kg. The conditioning regimens used were CHOP (cyclophosphamide, anthracycline, vincristine, and prednisone)-like, CBV (cyclophosphamide, carmustine, and etoposide), BEAM (carmustine, etoposide, cytarabine, and melphalan), and BEAC (carmustine, etoposide, cytarabine, and cyclophosphamide). For patients with bone marrow involvement at diagnosis, flow cytometry was performed before transplantation to detect lymphoma cells in bone marrow samples and/or apheresis grafts, and patients with positive results did not proceed to autologous transplantation. Written informed consent was obtained from all patients before transplantation.
DATA COLLECTION:
Demographic data, clinical characteristics, and laboratory parameters were collected through reviewing the medical records of all included patients. Histological subtype was determined according to the 2008 World Health Organization classification of lymphoid neoplasms [14]. The disease stage was evaluated based on the Ann Arbor staging system [15]. The presence of B symptoms included fever, night sweats, and weight loss. The international prognostic index (IPI) score at diagnosis was calculated based on age, disease stage, serum level of lactate dehydrogenase (LDH), number of extranodal disease sites, and ECOG PS [16]. Four risk groups were defined: low-risk group with IPI score of 0 to 1, low-intermediate-risk group with IPI score of 2, high-intermediate-risk group with IPI score of 3, and high-risk group with IPI score of 4 to 5. Remission status prior to ASCT was assessed by computed tomography (CT) scan. Complete remission (CR) was defined as the complete disappearance of evidence of disease, and partial remission (PR) was defined as at least a 50% decrease in the sum of the product of the diameters of up to 6 of the largest dominant nodes or nodal masses [17]. The level of serum albumin and other laboratory parameters before the initiation of conditioning chemotherapy were collected. Post-transplantation data of blood cell count were reviewed to assess engraftment; successful engraftment was defined as an absolute neutrophil count >0.5×106/L for 3 consecutive days [18].
The primary endpoint of this analysis was progression-free survival (PFS). Relapse or disease progression was defined as the appearance of any new lesion larger than 1.5 cm or a ≥50% increase of previously involved sites [17]. PFS was defined as time from the day of stem cell infusion to the first documented relapse, disease progression, or death from any cause. The second endpoint was overall survival (OS), which was defined as the time from day of stem cell infusion to death from any cause. Patients who were alive without progression were censored at the time of the last record or last contact.
STATISTICAL ANALYSIS:
All statistical analyses were performed with SPSS version 23.0 (IBM, Armonk, NY, USA). The cutoff value of albumin was 37 g/L, as previously established [19,20]. Demographic variables and disease characteristics were analyzed descriptively, and the differences between the low-albumin group and the high-albumin group were compared using the chi-squared test or Fisher’s exact test for categorical variables and the Wilcoxon test for continuous variables. PFS and OS were analyzed with the Kaplan-Meier method and compared with the log-rank test. Receiver operating characteristic (ROC) curve analysis was performed to explore the predictive value of serum albumin level on progression. Univariate and multivariate Cox proportional hazard regression analyses for PFS and OS were performed to identify potential prognostic factors. All reported P values are two-sided. A P value < 0.05 was considered to be statistically significant.
Results
PATIENT CHARACTERISTICS:
A total of 113 patients with lymphoma who received HDT/ASCT from peripheral blood stem cells at our center between January 2006 and August 2019 were included in this study. The median patient age at transplantation was 40 years (range, 4–68 years). There were 71 men and 42 women, with a ratio of 1.69. There were 80 patients diagnosed with B-cell NHL, including DLBCL (n=57), extranodal marginal zone lymphoma of mucosa-associated lymphoid tissue (MALT lymphoma, n=9), follicular lymphoma (n=4), primary mediastinal large B-cell lymphoma (n=2), mantle cell lymphoma (n=2), nodal marginal zone lymphoma (n=2), splenic B-cell lymphoma (n=1), T-cell/histiocyte-rich large B-cell lymphoma (n=1), ALK+ large B-cell lymphoma (n=1), and unclassifiable B-cell lymphoma with features intermediate between DLBCL and Burkitt lymphoma (n=1). There were 15 patients diagnosed with T-cell lymphoma, including ALK+ anaplastic large-cell lymphoma (n=5), ALK– anaplastic large-cell lymphoma (n=3), T-cell prolymphocytic leukemia (n=4), primary cutaneous anaplastic large-cell lymphoma (n=1), angioimmunoblastic T-cell lymphoma (n=1), and peripheral T-cell lymphoma (n=1). There were 4 patients diagnosed with extranodal NK/T-cell lymphoma, nasal type, and there were 14 patients with HL. Based on the Ann Arbor stage, most of the included patients (80.5%, 91/113) were diagnosed with advanced-stage disease (stage III–IV). An elevation of serum LDH level (>240 U/L) was observed in 44 patients (38.9%). All patients had received multiple cycles of chemotherapy before ASCT; the most commonly used regimens were CHOP for NHL and ABVD (doxorubicin, bleomycin, vinblastine, and dacarbazine) for HL. Of the 80 patients with B-cell NHL, 31 (38.8%) patients received rituximab combined with conventional chemotherapy. There were 54 patients who achieved CR and 57 patients who achieved PR before transplantation. The characteristics of all included patients are presented in Table 1.
TRANSPLANTATION OUTCOME:
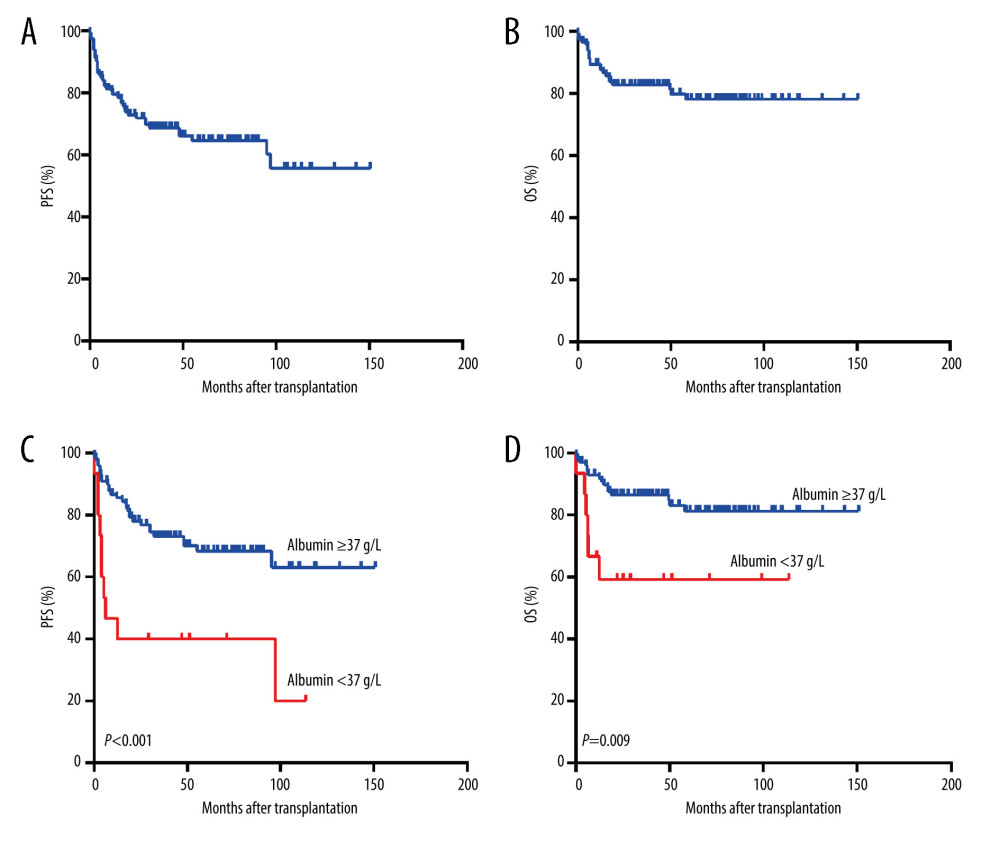
After being mobilized with granulocyte colony-stimulating factor alone or in combination with chemotherapy, all patients reached the peripheral blood stem cell collection target (>2×106 CD34+ cells/kg or >3×108 mononuclear cells/kg). The conditioning regimens applied were CHOP-like (n=27), CBV (n=30), BEAM (n=23), and BEAC (n=31). In addition, 1 patient received total body irradiation and cyclophosphamide, and 1 patient received busulfan and cyclophosphamide. Following the conditioning regimens, a median dose of 5.27×108 mononuclear cells/kg were infused. Except for 1 patient who died of severe pulmonary infection and 1 patient who died of acute hepatic failure before engraftment, all patients engrafted successfully. The median time to neutrophil engraftment was 11 days (range, 7–18 days). Post-ASCT maintenance therapies were given to 42 patients, including subcutaneous interferon alpha (IFN-α) (n=23), rituximab (n=7), cytokine-induced killer (CIK) cell infusion (n=7), and rituximab in combination with CIK cells (n=5). After a median follow-up of 49 months (range, 0.1–150.7 months), 23 patients died. The 3-year PFS and 3-year OS were 68.7% and 82.8%. The 5-year PFS and 5-year OS were 64.6% and 78.2%. The median PFS and median OS were not reached (Figure 1A, 1B). Patients who failed to achieved CR before transplantation were associated with inferior PFS and OS, but the differences were not statistically significant (P>0.05).
PROGNOSTIC ROLE OF SERUM ALBUMIN LEVEL:
The median serum level of albumin before transplantation was 41.3 g/L (range, 27.1–53.6 g/L). Based on the serum levels of albumin, we classified patients into a high-albumin (≥37 g/L) group and a low-albumin group (<37 g/L). Except for a higher proportion of patients who experienced LDH elevation (P=0.024) and a lower proportion of patients who achieved CR (P=0.026) in the low-albumin group, the patient characteristics were not significantly different between the 2 groups (P>0.05). Survival analyses indicated that the low-albumin group had significantly inferior PFS and OS (P<0.01) (Figure 1C, 1D). The 3-year PFS after transplantation was 76.8% in the high-albumin group and 40.0% in the low-albumin group (P=0.001). The 3-year OS after transplantation was 86.4% in the high-albumin group and 59.3% in the low-albumin group (P=0.009). The incidences of early progression (progressed within 1 year after transplantation) were 53.3% in the low-albumin group and 14.3% in the high-albumin group. Serum albumin level significantly predicted early progression, with an area under curve (AUC) of 0.706 (P=0.003). Low albumin (<37 g/L) significantly predicted early progression, with a sensitivity of 63.6% and a specificity of 92.3% (AUC=0.643, P=0.037).
OTHER PROGNOSTIC FACTORS:
To further investigate the prognostic role of albumin and other factors, we performed Cox proportional hazard regression analysis for PFS and OS. Univariate analysis showed that a low albumin level before transplantation (hazard ratio [HR] 3.29, 95% confidence interval [CI] 1.60–6.79; P=0.001), total protein level <60 g/L (HR 2.25, 95% CI 1.07–4.76; P=0.033), and age >60 years (HR 3.06, 95% CI 1.34–6.97; P=0.008) were significant risk factors for PFS. Sex, body mass index (BMI), lymphoma subtype, ECOG PS score, Ann Arbor stage, B symptoms, IPI risk score, LDH elevation, bone marrow involvement, disease duration from diagnosis to transplantation, number of prior regimens, disease status, globulin level, albumin/globulin ratio, conditioning regimens, dose of infused mononuclear cells, and maintenance therapy were not significantly associated with PFS (P>0.05). Multivariate analysis indicated that low albumin level before transplantation (HR 3.19, 95% CI 1.54–6.63; P=0.002) and age >60 years (HR 2.92, 95% CI 1.27–6.71; P=0.012) were independent risk factors for PFS. The results of univariate and multivariate analyses for PFS are shown in Table 2. For OS, univariate analysis suggested that low albumin (HR 3.29, 95% CI 1.28–8.46; P=0.013) and TP <60 g/L (HR 3.57, 95% CI 1.45–8.78; P=0.006) were associated with inferior OS; multivariate analysis indicated that TP < 60 g/L was an independent risk factor (HR 3.57, 95% CI 1.45–8.78; P=0.006; Table 3).
Since most of the included patients (70.8%) were diagnosed with B-cell NHL, we performed additional Cox regression analyses in this subgroup of patients. Univariate analysis showed that age >60 years (HR 3.37, 95% CI 1.41–8.06; P=0.006), high IPI risk (HR 3.39, 95% CI 1.13–10.18; P=0.029), LDH elevation (HR 2.52, 95% CI 1.18–5.40; P=0.017), bone marrow involvement (HR 3.09, 95% CI 1.16–8.24; P=0.024), disease status of PR or NR before transplantation (HR 2.65, 95% CI 1.21–5.80; P=0.015), albumin <37 g/L (HR 3.29, 95% CI 1.47–7.37, P=0.004), and TP <60 g/L (HR 2.81, 95% CI 1.26–6.27; P=0.012) were significantly associated with poorer PFS (Table 4). LDH elevation (HR 3.29, 95% CI 1.19–9.09; P=0.021), bone marrow involvement (HR 4.84, 95% CI 1.55–15.11; P=0.007), and TP <60 g/L (HR 4.65, 95% CI 1.72–12.59; P=0.002) were significantly associated with poorer OS (Table 5). Multivariate analysis indicated that age >60 years (HR 4.06, 95% CI 1.67–9.86, P=0.002) and albumin <37 g/L (HR 3.22, 95% CI 1.42–7.29; P=0.005) were independent risk factors for PFS; TP <60 g/L (HR 3.74, 95% CI 1.35–10.38; P=0.011) and LDH elevation (HR 2.83, 95% CI 1.003–8.01; P=0.049) were independent risk factors for OS.
Discussion
The major finding of this study was that low serum albumin level before transplantation was a valuable prognostic factor in patients with lymphoma undergoing HDT/ASCT. Low albumin levels in patients were associated with significantly inferior PFS and OS after transplantation. In addition, the serum level of albumin before transplantation predicted disease progression within 1 year after HDT/ASCT. Low albumin (<37 g/L) significantly predicted early progression with a high specificity of 92.3%. Moreover, multivariate analyses indicated that low albumin and age >60 years were independent risks factor for PFS and low TP was an independent risk factor for OS in the B-NHL subgroup and in the entire cohort.
To the best of our knowledge, this is the first study exploring the prognostic value of serum albumin levels before transplantation in patients with lymphoma undergoing HDT/ASCT. Multiple retrospective studies reported that low pretreatment albumin levels (lower than 3.5 g/dL or 3.7g/dL) are associated with poorer PFS and OS in patients with DLBCL, mantle cell lymphoma (MCL), peripheral T-cell lymphoma, and HL treated with conventional chemotherapy or immunochemotherapy [12,20–24]. In patients with a low or low-intermediate IPI-risk lymphoma, serum albumin levels at diagnosis could identify a subgroup of patients with remarkably better outcomes, in whom the 5-year OS is higher than 90%, indicating that albumin level is a useful prognostic factor that could improve the IPI-risk stratification [13,25]. Above all, the prognostic value of serum albumin level at diagnosis has been well established. However, the serum levels of albumin change during treatment. For example, in patients diagnosed with DLBCL and treated with R-CHOP (rituximab, cyclophosphamide, doxorubicin, vincristine, and prednisone), the serum levels of albumin were significantly different between cycle 1 and cycle 2 [26]. In our cohort, patients with refractory disease who received more cycles of chemotherapy had lower levels of albumin before transplantation. Until now, the prognostic role of pre-transplantation albumin level in patients undergoing HDT/ASCT has been unclear. The results of our present study showed that low pre-transplantation albumin levels were associated with extremely poor outcome after HDT/ASCT, suggesting that caution should be used in scheduling these patients for HDT/ASCT. Intensive care, nutritional support, and effective maintenance therapy after transplantation are required for these patients.
The possible mechanisms by which pre-transplantation albumin level predicted inferior outcome are as follows: low albumin levels are associated with poor nutritional status, more aggressive disease, repeated exposure to the toxicity of anti-tumor therapy, and decreased tolerance for high-dose conditioning regimens. Undermined tolerability from malnutrition is a common concern in patients with advanced malignancies. Previous studies have reported that malnourished patients with lymphoma identified by low serum albumin level or low BMI showed increased risk of chemotherapy-related complications and inferior treatment outcomes [27–29]. Our study failed to identify any significant association between BMI and post-transplantation outcome, suggesting that compared with BMI, albumin level would be a more sensitive parameter to reflect nutritional status in patients who have received multiple chemotherapy regimens. The serum albumin level is regulated by the rate of synthesis, degradation, and transvascular distribution [30]. It has been reported that the rate of albumin synthesis and transcapillary escape are similar in healthy individuals and patients with cancer, but the inflammatory response present in patients with advanced malignancies causes progressive loss of albumin [31,32]. Therefore, in addition to predicting the malnutrition status of a patient, a low albumin level may play a more important role in reflecting a more aggressive phenotype of the disease.
A low serum level of TP before transplantation is also a predictor of inferior outcome after ASCT in patients with lymphoma. Our results of Cox regression analyses show that TP <60 g/L was an independent risk factor of death, but no statistically significant association was found between TP level and PFS. A previous study suggested that TP is a superior predictor for survival than albumin in patients with lymphoma [33]. TP and albumin are commonly used laboratory parameters that are relatively convenient to collect in clinical practice. The integration of albumin with TP could be more helpful for outcome prediction after ASCT. Moreover, our data showed that age was a prognostic factor in patients with lymphoma undergoing ASCT. In our cohort, patients with age >60 years had significantly poorer outcomes than did younger patients, which is consistent with the results from another retrospective study [34]. Since the feasibility and efficacy of ASCT in selected elderly patients with lymphoma were established, the number of transplants in elderly patients has continuously increased over the past 2 decades [35–38]. Advanced age is no longer considered a contraindication for ASCT. However, older patients do have an increased incidence of complications and higher transplantation-related mortality [39]. Therefore, the selection of elderly patients for HDT/ASCT should be done cautiously, and, to improve survival, particular supportive care after ASCT is required for elderly patients with low serum levels of TP and albumin. Our study did not identify a statistically significant association between IPI score and survival outcomes after HDT/ASCT, which is consistent with the results of several previously published studies [40–42]. These combined results indicate that ASCT can overcome the disadvantageous effect of high-IPI risk on the survival of patients with lymphoma. The reason may be that the improvements of outcomes following hematopoietic stem cell transplantation are more distinguished in patients with high-IPI risk [4].
In addition to the above-mentioned parameters, we also investigated the prognostic role of different conditioning regimens and the use of rituximab. Our results suggested that the differences in conditioning regimens did not significantly affect PFS and OS after ASCT in patients with lymphoma, which is similar to the results from several other retrospective studies [43,44]. The choice of conditioning regimens for patients with lymphoma is largely dependent on institutional experience, and studies comparing the effects of different regimens have had prominent heterogeneity in study design, with often inconsistent results [45]. The optimal conditioning regimens for patients with different subtypes of lymphoma still need to be investigated in well-designed studies. In addition, only 38.8% patients with B-cell lymphoma in our cohort received rituximab during induction therapy, and our results of subgroup analyses suggested that rituximab induction was not a significant prognostic factor for PFS or OS in patients undergoing HDT/ASCT, which is consistent with the results of some retrospective studies from other centers [34,42]. The reason can be due to the heterogeneity in patient characteristics in our study, which resulted from the retrospective design, and the subgroup of patients receiving rituximab during induction therapy may have had more aggressive subtypes and higher risk of disease. Moreover, the significant improvements in survival outcomes with HDT/ASCT may offset the differences in prognosis from rituximab use. Since the proportions of patients receiving different conditioning regimens and receiving rituximab during induction therapy were not significantly different between the low-albumin group and the high-albumin group and the multivariate Cox regression analysis indicated that low albumin level was an independent risk factor, the differences in conditioning regimens and rituximab use did not affect our results and conclusions.
The value of post-transplant maintenance therapy in patients with lymphoma undergoing ASCT differs based on the disease subtypes and agents applied. In our cohort, rituximab, IFN-α, or CIK cells were used as maintenance therapy in a subgroup of patients, but the results of Cox regression analysis did not show any significant improvements in PFS and OS. A series of randomized controlled trials showed that rituximab maintenance therapy after ASCT significantly improved PFS in patients with rituximab-naïve, chemo-sensitive FL and MCL without evidence of rituximab resistance but did not significantly affect survival outcomes in patients with relapse or refractory DLBCL [9,10,46,47]. For patients with HL, consolidation with brentuximab vedotin after ASCT significantly prolonged PFS [11]. Based on this evidence, an expert panel from 3 leading international organizations in the field of hematopoietic cell transplantation recommended post-ASCT rituximab maintenance in patients with rituximab-naïve FL and MCL undergoing upfront ASCT and recommended brentuximab vedotin maintenance/consolidation in high-risk HL; however, no post-transplantation maintenance was recommended for DLBCL [48]. Although the combination of IFN-α or CIK cells with traditional chemotherapy was reported to improve treatment outcomes in patients with lymphoma, results from a randomized controlled trial suggested that post-ASCT IFN-α did not improve outcomes, and, to the best of our knowledge, no randomized controlled trials investigating the effects of post-ASCT CIK-cell maintenance have been conducted [49–51]. Bortezomib maintenance after ASCT in patients with MCL also did not show any significant improvements [52]. Therefore, the offer of post-ASCT therapies with new agents is recommended only in clinical trials [48]. Additional well-designed prospective studies are required to establish the value and the optimal regimen of post-ASCT maintenance therapy.
Conclusions
In conclusion, for patients with lymphoma undergoing HDT/ASCT, low serum albumin level before transplantation was found to be an independent prognostic factor predicting poor outcome. For decision-making in clinical practice, it should be considered that patients with low albumin levels may not benefit from HDT/ASCT as much as would patients with normal albumin levels. Intensive care, nutritional support, and effective maintenance therapy may be helpful in improving post-transplantation outcomes for these patients.
Tables
Table 1. Characteristics of included patients.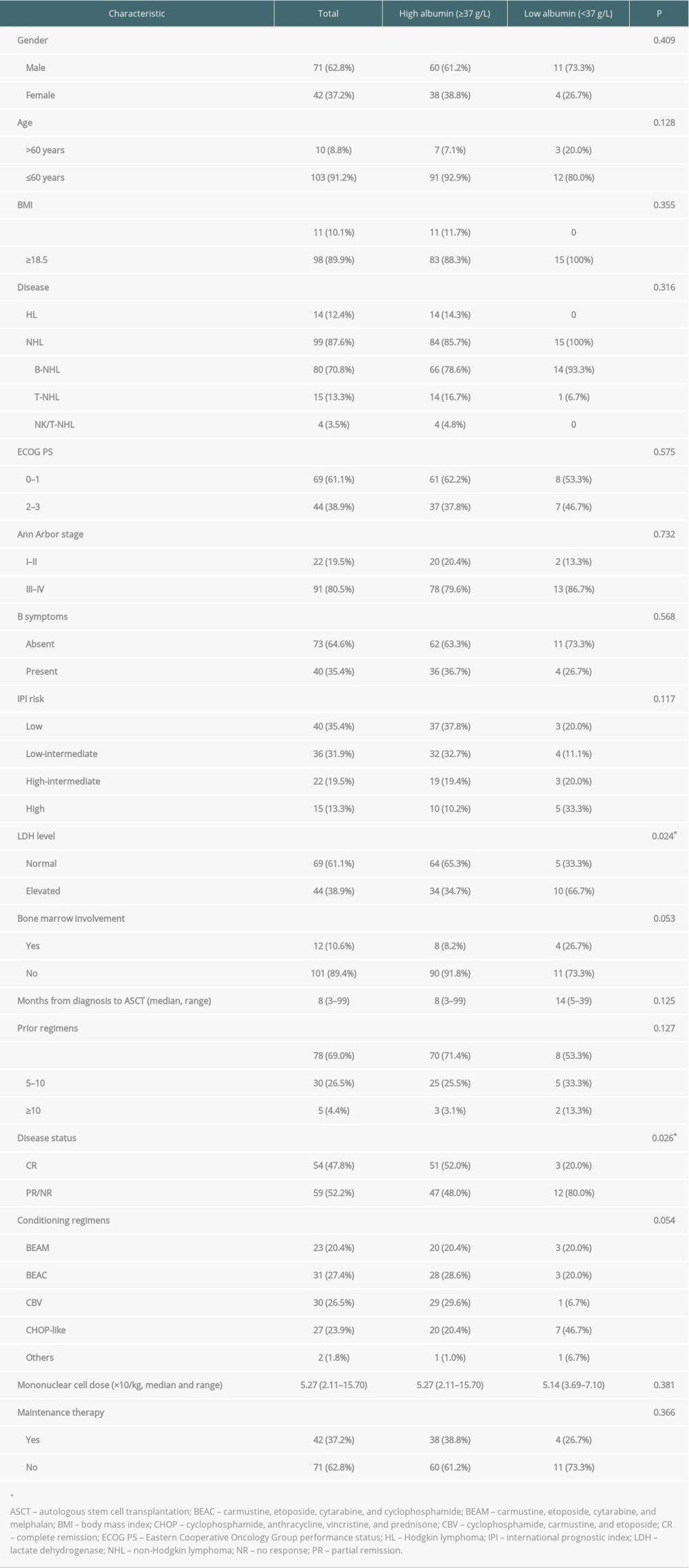 Table 2. Results of univariate and multivariate Cox regression analyses for progression-free survival.
Table 2. Results of univariate and multivariate Cox regression analyses for progression-free survival.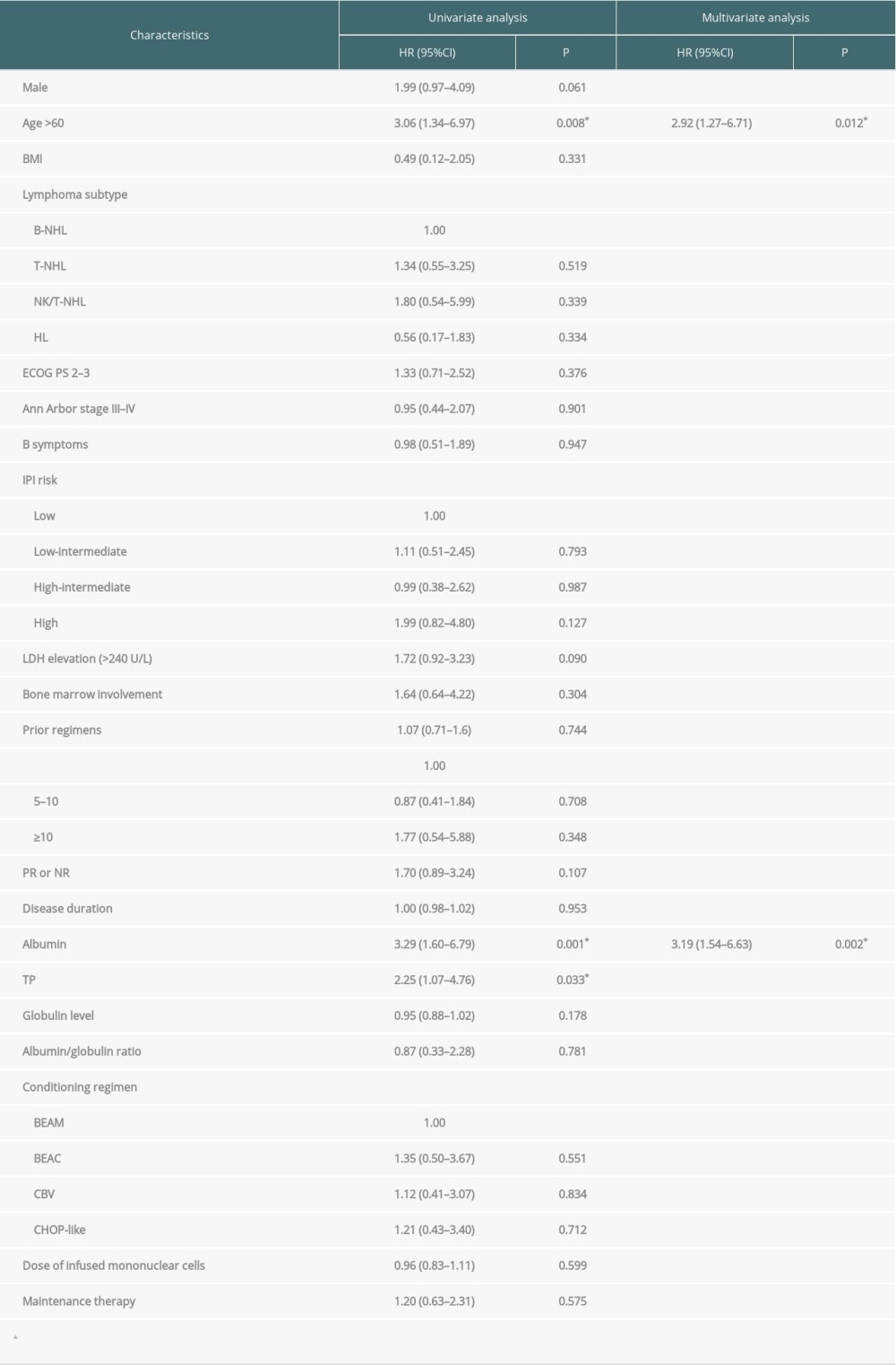 Table 3. Results of univariate and multivariate Cox regression analyses for overall survival.
Table 3. Results of univariate and multivariate Cox regression analyses for overall survival.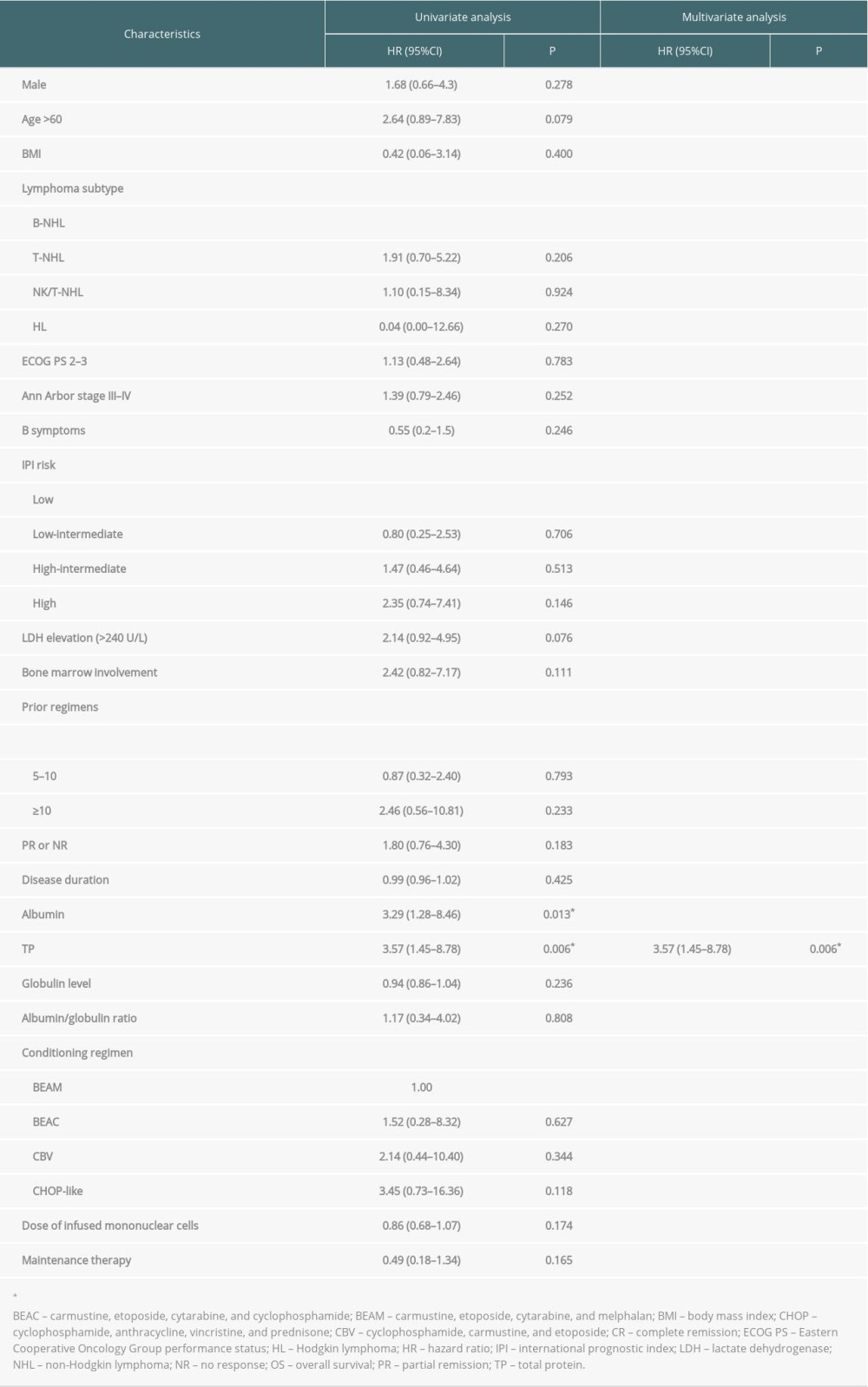 Table 4. Results of univariate and multivariate Cox regression analyses for progression-free survival in the B-cell non-Hodgkin lymphoma subgroup.
Table 4. Results of univariate and multivariate Cox regression analyses for progression-free survival in the B-cell non-Hodgkin lymphoma subgroup.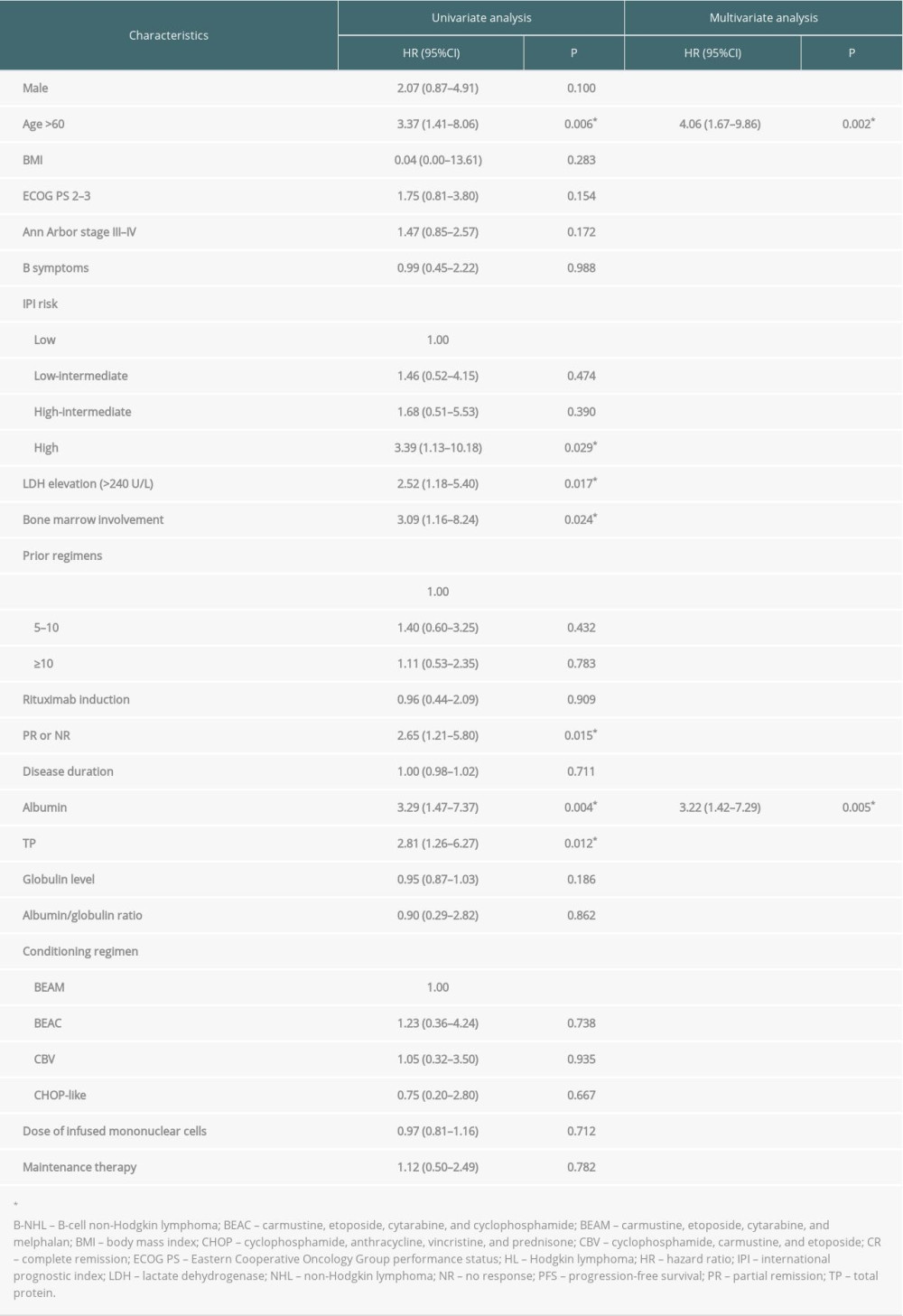 Table 5. Results of univariate and multivariate Cox regression analyses for overall survival in the B-cell non-Hodgkin lymphoma subgroup.
Table 5. Results of univariate and multivariate Cox regression analyses for overall survival in the B-cell non-Hodgkin lymphoma subgroup.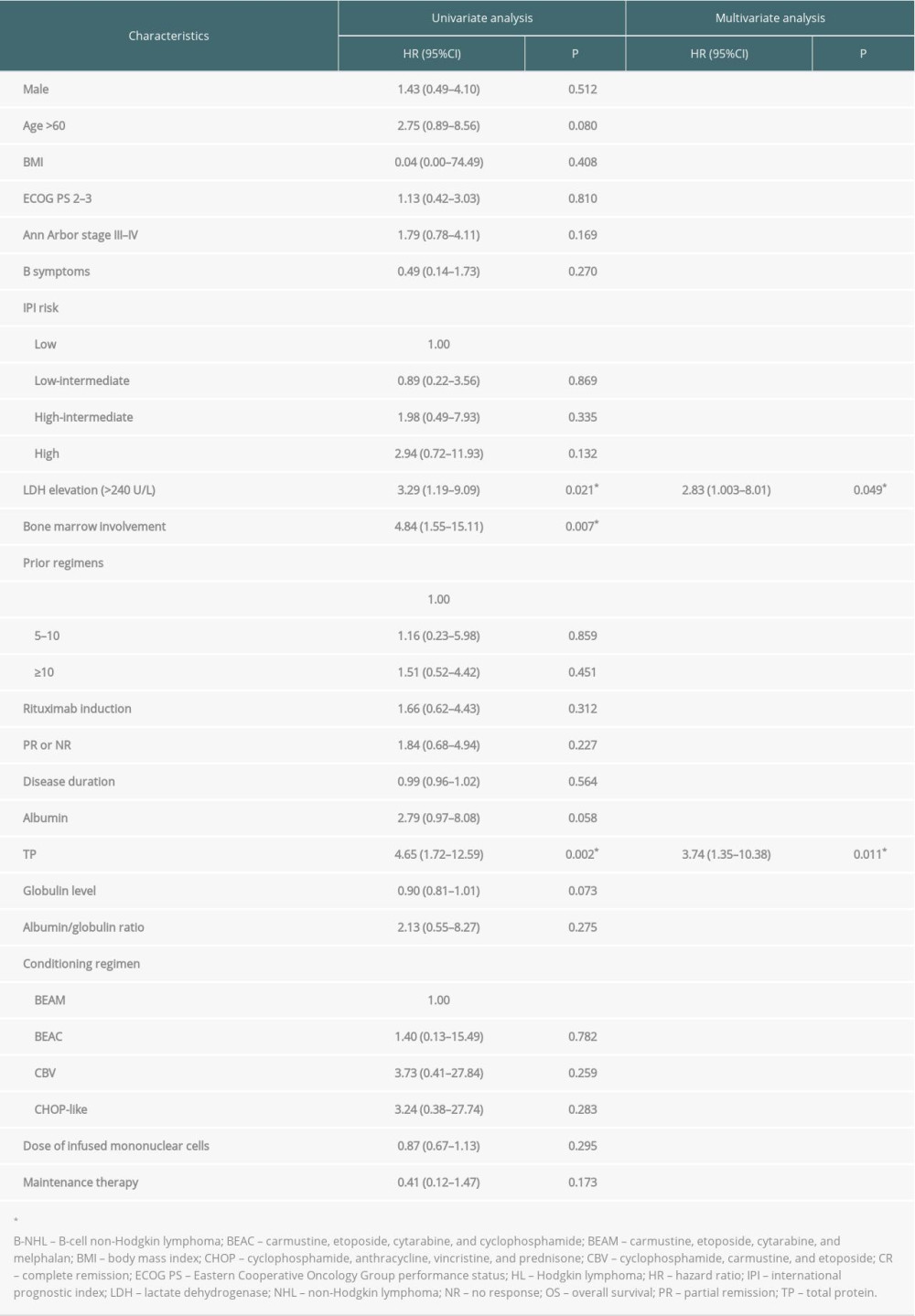
References
1. Bray F, Ferlay J, Soerjomataram I, Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries: Cancer J Clin, 2018; 68(6); 394-424
2. Coiffier B, Lepage E, Briere J, CHOP chemotherapy plus rituximab compared with CHOP alone in elderly patients with diffuse large-B-cell lymphoma: N Engl J Med, 2002; 346(4); 235-42
3. Chen R, Palmer JM, Martin P, Results of a multicenter phase ii trial of brentuximab vedotin as second-line therapy before autologous transplantation in relapsed/refractory hodgkin lymphoma: Biol Blood Marrow Transplant, 2015; 21(12); 2136-40
4. Stiff PJ, Unger JM, Cook JR, Autologous transplantation as consolidation for aggressive non-Hodgkin’s lymphoma: N Engl J Med, 2013; 369(18); 1681-90
5. Chiappella A, Martelli M, Angelucci E, Rituximab-dose-dense chemotherapy with or without high-dose chemotherapy plus autologous stem-cell transplantation in high-risk diffuse large B-cell lymphoma (DLCL04): Final results of a multicentre, open-label, randomised, controlled, phase 3 study: Lancet Oncol, 2017; 18(8); 1076-88
6. Schmitz N, Pfistner B, Sextro M, Aggressive conventional chemotherapy compared with high-dose chemotherapy with autologous haemopoietic stem-cell transplantation for relapsed chemosensitive Hodgkin’s disease: A randomised trial: Lancet, 2002; 359(9323); 2065-71
7. Philip T, Guglielmi C, Hagenbeek A, Autologous bone marrow transplant as compared with salvage chemotherapy in relapses of chemotherapy-sensitive non-Hodgkin’s lymphoma: N Engl J Med, 1995; 333(23); 1540-45
8. Epperla N, Fenske TS, Lazarus HM, Post-autologous transplant maintenance therapies in lymphoid malignancies: Are we there yet?: Bone Marrow Transplant, 2015; 50(11); 1393-404
9. Le Gouill S, Thieblemont C, Oberic L, Rituximab after autologous stem-cell transplantation in mantle-cell lymphoma: N Engl J Med, 2017; 377(13); 1250-60
10. Pettengell R, Schmitz N, Gisselbrecht C, Rituximab purging and/or maintenance in patients undergoing autologous transplantation for relapsed follicular lymphoma: A prospective randomized trial from the Lymphoma Working Party of the European Group for Blood and Marrow Transplantation: J Clin Oncol, 2013; 31(13); 1624-30
11. Moskowitz CH, Nademanee A, Masszi T, Brentuximab vedotin as consolidation therapy after autologous stem-cell transplantation in patients with Hodgkin’s lymphoma at risk of relapse or progression (AETHERA): A randomised, double-blind, placebo-controlled, phase 3 trial: Lancet, 2015; 385(9980); 1853-62
12. Bairey O, Shacham-Abulafia A, Shpilberg O, Gurion R, Serum albumin level at diagnosis of diffuse large B-cell lymphoma: An important simple prognostic factor: Hematol Oncol, 2016; 34(4); 184-92
13. Wei Y, Wei X, Huang W, Albumin improves stratification in the low IPI risk patients with diffuse large B-cell lymphoma: Int J Hematol, 2020; 111(5); 681-85
14. Campo E, Swerdlow SH, Harris NL, The 2008 WHO classification of lymphoid neoplasms and beyond: Evolving concepts and practical applications: Blood, 2011; 117(19); 5019-32
15. Rosenberg SA, Validity of the Ann Arbor staging classification for the non-Hodgkin’s lymphomas: Cancer Treat Rep, 1977; 61(6); 1023-27
16. International Non-Hodgkin’s Lymphoma Prognostic Factors Project, A predictive model for aggressive non-Hodgkin’s lymphoma: N Engl J Med, 1993; 329(14); 987-94
17. Cheson BD, Pfistner B, Juweid ME, Revised response criteria for malignant lymphoma: J Clin Oncol, 2007; 25(5); 579-86
18. Yuan S, Palmer JM, Tsai NC, Engraftment and outcomes following autologous stem cell transplantation in Hodgkin lymphoma patients mobilized with plerixafor: Hematol Oncol, 2017; 35(3); 281-87
19. Ngo L, Hee SW, Lim LC, Prognostic factors in patients with diffuse large B cell lymphoma: Before and after the introduction of rituximab: Leuk Lymphoma, 2008; 49(3); 462-69
20. Dalia S, Chavez J, Little B, Serum albumin retains independent prognostic significance in diffuse large B-cell lymphoma in the post-rituximab era: Ann Hematol, 2014; 93(8); 1305-12
21. Chihara D, Asano N, Ohmachi K, Prognostic model for mantle cell lymphoma in the rituximab era: A nationwide study in Japan: Br J Haematol, 2015; 170(5); 657-68
22. Chihara D, Oki Y, Ine S, Analysis of prognostic factors in peripheral T-cell lymphoma: Prognostic value of serum albumin and mediastinal lymphadenopathy: Leuk Lymphoma, 2009; 50(12); 1999-2004
23. Kılıçkap S, Barışta I, Ulger S, Clinical features and prognostic factors of Hodgkin’s lymphoma: A single center experience: Balkan Med J, 2013; 30(2); 178-85
24. Hasenclever D, Diehl V, A prognostic score for advanced Hodgkin’s disease. International Prognostic Factors Project on Advanced Hodgkin’s Disease: N Engl J Med, 1998; 339(21); 1506-14
25. Melchardt T, Troppan K, Weiss L, A modified scoring of the NCCN-IPI is more accurate in the elderly and is improved by albumin and β2-microglobulin: Br J Haematol, 2015; 168(2); 239-45
26. Eatrides J, Thompson Z, Lee JH, Serum albumin as a stable predictor of prognosis during initial treatment in patients with diffuse large B cell lymphoma: Ann Hematol, 2015; 94(2); 357-58
27. Park S, Han B, Cho JW, Effect of nutritional status on survival outcome of diffuse large B-cell lymphoma patients treated with rituximab-CHOP: Nutr Cancer, 2014; 66(2); 225-33
28. Kanemasa Y, Shimoyama T, Sasaki Y, Analysis of the prognostic value of BMI and the difference in its impact according to age and sex in DLBCL patients: Hematol Oncol, 2018; 36(1); 76-83
29. Li YJ, Yi PY, Li JW, Increased body mass index is associated with improved overall survival in extranodal natural killer/T-cell lymphoma, nasal type: Oncotarget, 2017; 8(3); 4245-56
30. Nicholson JP, Wolmarans MR, Park GR, The role of albumin in critical illness: Br J Anaesth, 2000; 85(4); 599-610
31. McMillan DC, Watson WS, O’Gorman P, Albumin concentrations are primarily determined by the body cell mass and the systemic inflammatory response in cancer patients with weight loss: Nutr Cancer, 2001; 39(2); 210-13
32. Barbosa-Cortés L, Klunder-Klunder M, López-Alarcón M, Nutritional status and cytokine concentration during chemotherapy in Mexican children: A longitudinal analysis: Nutrition, 2019; 57; 46-51
33. Watanabe T, Kinoshita T, Itoh K, Pretreatment total serum protein is a significant prognostic factor for the outcome of patients with peripheral T/natural killer-cell lymphomas: Leuk Lymphoma, 2010; 51(5); 813-21
34. Armand P, Welch S, Kim HT, Prognostic factors for patients with diffuse large B cell lymphoma and transformed indolent lymphoma undergoing autologous stem cell transplantation in the positron emission tomography era: Br J Haematol, 2013; 160(5); 608-17
35. Jantunen E, Itälä M, Juvonen E, Autologous stem cell transplantation in elderly (>60 years) patients with non-Hodgkin’s lymphoma: A nation-wide analysis: Bone Marrow Transplant, 2006; 37(4); 367-72
36. Buadi FK, Micallef IN, Ansell SM, Autologous hematopoietic stem cell transplantation for older patients with relapsed non-Hodgkin’s lymphoma: Bone Marrow Transplant, 2006; 37(11); 1017-22
37. Dahi PB, Tamari R, Devlin SM, Favorable outcomes in elderly patients undergoing high-dose therapy and autologous stem cell transplantation for non-Hodgkin lymphoma: Biol Blood Marrow Transplant, 2014; 20(12); 2004-9
38. Dogu MH, Çagirgan S, Ocakci S, Autologous stem cell transplantation and stem cell mobilization kinetics in elderly patients with B cell non-Hodgkin lymphoma: Transfus Apher, 2017; 56(6); 814-18
39. Lazarus HM, Carreras J, Boudreau C, Influence of age and histology on outcome in adult non-Hodgkin lymphoma patients undergoing autologous hematopoietic cell transplantation (HCT): A report from the Center For International Blood & Marrow Transplant Research (CIBMTR): Biol Blood Marrow Transplant, 2008; 14(12); 1323-33
40. Lee HG, Choi Y, Kim SY, R-CHOP chemoimmunotherapy followed by autologous transplantation for the treatment of diffuse large B-cell lymphoma: Blood Res, 2014; 49(2); 107-14
41. Roerden M, Walz JS, The role of autologous stem cell transplantation in peripheral T cell lymphoma: A long-term follow-up single-center experience: J Cancer Res Clin Oncol, 2019; 145(10); 2595-604
42. Kriegsmann K, Rieger M, Schwarzbich MA, Outcome after high-dose chemotherapy and autologous stem cell transplantation in patients with aggressive B-cell non-Hodgkin’s lymphoma: Eur J Haematol, 2018; 101(1); 12-20
43. Shi Y, Liu P, Zhou S, Comparison of CBV, BEAM and BEAC high-dose chemotherapy followed by autologous hematopoietic stem cell transplantation in non-Hodgkin lymphoma: Efficacy and toxicity: Asia-Pac J Clin Oncol, 2017; 13(5); e423-e9
44. Huang H, Zhang L, Jiang Y, Modified BuCy is an alternative conditioning regimen for lymphoma patients undergoing autologous stem cell transplantation: Ann Hematol, 2019; 98(5); 1259-66
45. Chen YB, Lane AA, Logan B, Impact of conditioning regimen on outcomes for patients with lymphoma undergoing high-dose therapy with autologous hematopoietic cell transplantation: Biol Blood Marrow Transplant, 2015; 21(6); 1046-53
46. Gisselbrecht C, Schmitz N, Mounier N, Rituximab maintenance therapy after autologous stem-cell transplantation in patients with relapsed CD20(+) diffuse large B-cell lymphoma: Final analysis of the collaborative trial in relapsed aggressive lymphoma: J Clin Oncol, 2012; 30(36); 4462-69
47. Haioun C, Mounier N, Emile JF, Rituximab versus observation after high-dose consolidative first-line chemotherapy with autologous stem-cell transplantation in patients with poor-risk diffuse large B-cell lymphoma: Ann Oncol, 2009; 20(12); 1985-92
48. Kanate AS, Kumar A, Dreger P, Maintenance therapies for Hodgkin and non-Hodgkin lymphomas after autologous transplantation: A Consensus Project of ASBMT, CIBMTR, and the Lymphoma Working Party of EBMT: JAMA Oncol, 2019; 5(5); 715-22
49. Rohatiner AZ, Gregory WM, Peterson B, Meta-analysis to evaluate the role of interferon in follicular lymphoma: J Clin Oncol, 2005; 23(10); 2215-23
50. Zhou M, Wang J, Li CP, Autologous cytokine-induced killer cell immunotherapy for patients with high-risk diffuse large B cell lymphoma after the first complete remission: Onco Targets Ther, 2020; 13; 5879-85
51. Bosly A, Grigg A, Holte H, A randomized study of interferon α-2b versus no treatment as consolidation after high dose therapy and autologous stem cell transplantation for patients with relapsed lymphoma: Oncologist, 2013; 18(11); 1189
52. Doorduijn JK, Zijlstra JM, Lugtenburg PJ, Bortezomib maintenance after R-CHOP, cytarabine and autologous stem cell transplantation in newly diagnosed patients with mantle cell lymphoma, results of a randomised phase II HOVON trial: Br J Haematol, 2020; 190(3); 385-93
Tables
 Table 1. Characteristics of included patients.
Table 1. Characteristics of included patients. Table 2. Results of univariate and multivariate Cox regression analyses for progression-free survival.
Table 2. Results of univariate and multivariate Cox regression analyses for progression-free survival. Table 3. Results of univariate and multivariate Cox regression analyses for overall survival.
Table 3. Results of univariate and multivariate Cox regression analyses for overall survival. Table 4. Results of univariate and multivariate Cox regression analyses for progression-free survival in the B-cell non-Hodgkin lymphoma subgroup.
Table 4. Results of univariate and multivariate Cox regression analyses for progression-free survival in the B-cell non-Hodgkin lymphoma subgroup. Table 5. Results of univariate and multivariate Cox regression analyses for overall survival in the B-cell non-Hodgkin lymphoma subgroup.
Table 5. Results of univariate and multivariate Cox regression analyses for overall survival in the B-cell non-Hodgkin lymphoma subgroup. Table 1. Characteristics of included patients.
Table 1. Characteristics of included patients. Table 2. Results of univariate and multivariate Cox regression analyses for progression-free survival.
Table 2. Results of univariate and multivariate Cox regression analyses for progression-free survival. Table 3. Results of univariate and multivariate Cox regression analyses for overall survival.
Table 3. Results of univariate and multivariate Cox regression analyses for overall survival. Table 4. Results of univariate and multivariate Cox regression analyses for progression-free survival in the B-cell non-Hodgkin lymphoma subgroup.
Table 4. Results of univariate and multivariate Cox regression analyses for progression-free survival in the B-cell non-Hodgkin lymphoma subgroup. Table 5. Results of univariate and multivariate Cox regression analyses for overall survival in the B-cell non-Hodgkin lymphoma subgroup.
Table 5. Results of univariate and multivariate Cox regression analyses for overall survival in the B-cell non-Hodgkin lymphoma subgroup. In Press
18 Mar 2024 : Original article
Does Antibiotic Use Increase the Risk of Post-Transplantation Diabetes Mellitus? A Retrospective Study of R...Ann Transplant In Press; DOI: 10.12659/AOT.943282
20 Mar 2024 : Original article
Transplant Nephrectomy: A Comparative Study of Timing and Techniques in a Single InstitutionAnn Transplant In Press; DOI: 10.12659/AOT.942252
28 Mar 2024 : Original article
Association Between FEV₁ Decline Rate and Mortality in Long-Term Follow-Up of a 21-Patient Pilot Clinical T...Ann Transplant In Press; DOI: 10.12659/AOT.942823
02 Apr 2024 : Original article
Liver Transplantation from Brain-Dead Donors with Hepatitis B or C in South Korea: A 2014-2020 Korean Organ...Ann Transplant In Press; DOI: 10.12659/AOT.943588
Most Viewed Current Articles
05 Apr 2022 : Original article
Impact of Statins on Hepatocellular Carcinoma Recurrence After Living-Donor Liver TransplantationDOI :10.12659/AOT.935604
Ann Transplant 2022; 27:e935604
12 Jan 2022 : Original article
Risk Factors for Developing BK Virus-Associated Nephropathy: A Single-Center Retrospective Cohort Study of ...DOI :10.12659/AOT.934738
Ann Transplant 2022; 27:e934738
22 Nov 2022 : Original article
Long-Term Effects of Everolimus-Facilitated Tacrolimus Reduction in Living-Donor Liver Transplant Recipient...DOI :10.12659/AOT.937988
Ann Transplant 2022; 27:e937988
15 Mar 2022 : Case report
Combined Liver, Pancreas-Duodenum, and Kidney Transplantation for Patients with Hepatitis B Cirrhosis, Urem...DOI :10.12659/AOT.935860
Ann Transplant 2022; 27:e935860