12 August 2022: Original Paper
Retrospective Study from a Single Center in Romania of 347 Renal Transplant Patients Treated with Tacrolimus, Mycophenolate, and Steroids to Evaluate the Association Between Anti-HLA Antibodies and 5-Year Graft Survival
Ion Mărunţelu12ABCDEF, Claudiu Eduard NistorDOI: 10.12659/AOT.937267
Ann Transplant 2022; 27:e937267
Abstract
BACKGROUND: Kidney transplantation is the most recommended treatment in chronic kidney disease. The recipient’s immune system reacts to a kidney graft as to an alloantigen by producing antibodies (anti-human leukocyte antigens [HLAs]). Although immunosuppressive therapy is used to overcome this problem, the long-term survival of a kidney graft after 5 years remains low. This retrospective study from a single center in Romania of 347 renal transplant patients treated with tacrolimus, mycophenolate, and steroids aimed to evaluate the association between anti-HLA antibodies and 5-year graft survival.
MATERIAL AND METHODS: Anti-HLA antibodies were screened and identified using the Luminex method, while tacrolimus levels were monitored using the chemiluminescent assay.
RESULTS: Twenty-seven patients had pre-existing anti-HLA antibodies, while 320 patients did not. Of the 320 patients, 15% developed anti-HLA antibodies following kidney transplantation. The intrapatient minimum blood level of tacrolimus (cut-off value: 4.6 ng/mL) after transplantation was significantly associated with the risk of de novo anti-HLA antibodies (P<0.001). In patients with or without de novo anti-HLA antibodies, the 5-year allograft survival rate was 77.1% vs 90.8% (P=0.004). After Bonferroni correction, donor age (P=0.001), and donor type (P<0.0001) were statistically associated with the risk of allograft rejection.
CONCLUSIONS: This study showed that anti-HLA antibodies at 5 years after kidney transplantation were significantly associated with graft failure. The findings support previous studies and indicate that monitoring of anti-HLA antibodies should be considered in patients with renal transplant.
Keywords: Allografts, Graft Rejection, Graft Survival, HLA Antigens, Kidney Transplantation, Tacrolimus, Antilymphocyte Serum, Humans, Immunosuppressive Agents, Romania, Steroids
Background
Kidney transplantation significantly improves patient quality of life and allows socio-professional reintegration [1]. Kidney grafts can be transplanted either from brain-dead or living donors. Usually, kidney transplantation is possible when there is no anti-human leukocyte (HLA) donor-specific antibody incompatibility because of a high risk of hyperacute or acute kidney graft rejection [2–4]. However, this approach is associated with a reduced chance of highly immunized patients getting transplants that may prolong their life [5]. Orandi et al observed that patients with HLA incompatibility transplanted from living donors have a longer life expectancy than those who remain on a brain-dead donor waiting list [2]. In the case of transplantation with HLA incompatibility from a cadaveric donor, Krishnan et al have shown that long-term survival is similar to that of patients transplanted from brain-dead but HLA-matched donors [3].
Despite advances made in immunosuppressant development, not all patients have functional renal allografts after approximately 5 years [6]. The recipient’s immune system responds to the kidney transplant by producing anti-HLA antibodies, resulting in humoral rejection of the kidney allograft [7] and different outcomes in terms of graft survival rate [8–10]. Analyzing the dynamics of donor-specific anti-HLA antibodies in the immediate posttransplant period, Phillpott et al identified an increase in anti-HLA antibody levels in the first 2 weeks after kidney transplantation, followed by a slight decrease [10]. Reduction in anti-HLA antibodies could be due to strong immunosuppression, their clearance from the circulation by plasmapheresis [11], or prevention of CD20 B lymphocytes from turning into plasma cells using monoclonal antibodies, such as rituximab [12].
To avoid rejection, in addition to low-resolution HLA typing of both recipient and donor for all loci, pretransplantation screening for anti-HLA antibodies and the crossmatch test are performed [13,14]. Crossmatch, which is used to detect the presence of donor-specific alloantibodies in patients’ serum, eliminated the phenomenon of hyperacute renal allograft rejection but not chronic rejection [15]. Extensive anti-HLA antibody assessment allowed us to practice more virtual crossmatch in order to shorten the time [16].
Currently, Luminex technology is the most widely used method for the detection and identification of anti-HLA antibodies with high sensitivity (both before and after kidney transplantation) [17,18] and crossmatch testing (before kidney transplantation) [19]. Unlike enzyme-linked immunoassay, Luminex technology allows the simultaneous analysis of a very large number of analytes (up to several hundred) from a small sample volume, with applications in solid organ transplantation, hematopoietic stem cell transplantation, and transfusions [20], infectious diseases [21], autoimmune diseases [22], and cancer [23].
T-cell- and antibody-mediated rejection are 2 main histopathological findings in patients with graft rejection. While T-cell-mediated rejection has little effect on graft survival, antibody-mediated rejection presents microcirculation lesions because of mediated inflammatory cytokine, such as interferon gamma, affecting the graft functions [24].
In our opinion, the factors that influence kidney transplant outcomes are complex. Therefore, this retrospective study from a single center in Romania of 347 renal transplant patients treated with tacrolimus, mycophenolate, and steroids aimed to evaluate the association between anti-HLA antibodies and 5-year graft survival.
Material and Methods
METHODS:
Our research was undertaken with the approval of the Ethics Committee of the Fundeni Clinical Institute (no. 77883 from 2021), and written informed consent was obtained from all patients. According to the written informed consent, patients who agreed to be included in the present study were free to withdraw their consent without being charged, whenever they decided.
The presence of preformed and de novo anti-HLA antibodies was retrospectively analyzed in serum samples before transplantation and at 1 to 5 years after transplantation.
All the recipients had a compatible donor based on HLA genes. None of the recipients had preformed donor-specific antibodies.
Class I and class II HLA antibodies were screened with LABScreen Mixed12, lot 023 (One Lambda, Inc., Canoga Park, CA, USA) on FlexMap3d (Luminex Corporation, USA). The positive screening was followed by the identification of anti-HLA antibodies with LS1A04 lot 013 (for class I) and LS2A01 lot 014 (for class II) kits from One Lambda. Screening and identification of class I and class II HLA antibodies were carried out following the manufacturer guidelines, and sample data were collected using xPONENT software version 4.3 (Luminex Corporation, USA) [25] and analyzed with HLA Fusion version 4.3 (One Lambda, Inc.). Based on a mean fluorescence intensity cut-off value of 1500, the anti-HLA antibody was considered either positive or negative. The identified anti-HLA antibodies were then compared with the donor’s HLA, which allowed us to identify donor-specific antibodies and non-donor-specific antibodies. Also, we were able to specify if the identified HLA antibodies were preformed (formed before any kidney transplant) or de novo (appeared after a kidney transplant).
Tacrolimus levels in the blood were determined using tacrolimus reagent kits and a chemiluminescent magnetic microparticle immunoassay (Architect i2000, Abbot).
Acute or chronic graft rejection was identified by kidney biopsies that were analyzed based on the Banff criteria [26].
STATISTICAL ANALYSIS:
SPSS version 26 (IBM Corp, Armonk, NY, USA) was used for all statistical analyses. Categorical variables are presented as counts and percentages, while continuous variables are reported as means and standard deviations. For categorical and continuous variables, Fisher’s exact or the chi-square test were used to compare patients with kidney transplant characteristics in groups differentiated by the presence or absence of anti-HLA antibodies.
Variability of the blood level of tacrolimus was estimated by calculating the coefficient of variation using the following equation: coefficient of variation (%)=(standard deviation/mean concentration)×100 [27]. The cut-off values for the intrapatient minimum trough level of tacrolimus at 1 to 5 years after transplantation for predicting the production of anti-HLA antibodies were determined using receiver operating characteristic (ROC) curve analysis. Bonferroni correction was also applied in the case of multivariate analysis.
Data on transplant survival were recorded and stored until either the time of the patient’s death or graft loss. Kaplan-Meier analysis was used to plot the survival rates of renal grafts, and the log-rank test was used to compare the groups. A
Results
A total of 347 patients who underwent kidney transplantation between January 2013 and December 2016 were included in the analysis. Based on pre-existing HLA antibodies, all patients were divided into 2 groups: patients with pre-existing HLA antibodies and patients without pre-existing HLA antibodies. In both groups, chronic glomerulonephritis was the leading cause of chronic renal insufficiency.
In the group without HLA antibodies, 36.9% of patients were women, 63.1% were men, and the average age was 46.7±11.6 years. The follow-up period for the patients included in this group was 4.8±0.7 years. Most kidney grafts were obtained from living-related donors (62.8%).
In the group with previous HLA antibodies, 37.0% of patients were men, and 63.0% were women, with an average patient age of 40.7±12.7 years. The follow-up period for the patients included in this group was 3.4±1.4 years. Most kidney grafts were obtained from cadaveric donors (55.6%).
At 5 years after transplantation, 48 (15%) patients with kidney transplants had de novo anti-HLA antibodies (Table 1). Twenty-two (6.87%) patients had de novo class I anti-HLA antibodies. De novo class II anti-HLA antibodies were observed in 37 (13.07%) patients (Table 2).
As shown in Table 3, antibody-mediated rejection was observed in 10 (20.83%) of the 48 patients from the group with de novo anti-HLA antibodies and in 7 (25.93%) of the 27 patients from the group with pre-existing anti-HLA antibodies. T-cell-mediated rejection was diagnosed in 13 (48.15%) of the 27 patients from the group with pre-existing anti-HLA antibodies and in 19 (39.58%) of the 48 patients from the group with de novo anti-HLA antibodies. Analysis of the possible outcomes showed that T-cell-mediated rejection and antibody-mediated rejection were not related to de novo anti-HLA antibodies.
The association of tacrolimus blood level with de novo HLA antibody production and rejection was studied. The ROC test was used to determine the cut-off value of the tacrolimus blood level. Only a tacrolimus blood level lower than 4.6 ng/mL was associated with de novo HLA antibody positivity. The area under the ROC curve (used to determine the cut-off values of 4.6 ng/mL; Figure 1) was 0.85, with a 95% confidence interval (CI) of 0.80 to 0.88 and
We also analyzed the possible association of donor age, donor type, recipient age, and de novo HLA antibodies with kidney rejection in both groups. In patients without previous sensitization, only donor age (odds ratio [OR]=1.07,
In the groups of patients without previous anti-HLA antibodies, the death-censored renal graft survival rates were 95.8% vs 98.9% (1 year), 89.6% vs 97.1% (2 years), 85.4% vs 95.2% (3 years), 81.3% vs 92.6% (4 years), and 77.1% vs 90.8% (5 years) (Figure 3, Table 4). The graft survival rate was significantly lower in recipients with de novo anti-HLA antibodies 5 years after transplantation
In the groups of patients with previous anti-HLA antibodies, the death-censored renal graft survival rates were 96.3% (1 year), 92.6% (2 years), 88.9% (3 years), 77.8% (4 years), and 74.1% (5 years).
When comparing both patient groups, we observed that there was a significant difference between survival distributions 5 years after kidney transplantation (
Only 4 patients with previous anti-HLA antibodies and 8 patients without previous HLA sensitization developed donor-specific HLA antibodies after kidney transplantation. In our patients, there was no significant difference between survival distributions 5 years after kidney transplantation in patients with donor-specific antibodies and those without (
Discussion
After kidney transplantation, the incidence of patients with anti-HLA antibodies was relatively small (15%), similar to the incidence observed in a study of 2185 patients by Terasaki and Ozawa (14.7%) [28]. The administration of calcineurin inhibitors in the early posttransplantation period could protect against the development of de novo anti-HLA antibodies [29,30]. However, studies have shown that a lower tacrolimus trough level is associated with the development of de novo anti-HLA antibodies [29,31,32],
Marked intrapatient variability in tacrolimus trough levels may be a major risk factor for de novo anti-HLA antibodies [33–35]. In our clinical experience, the intrapatient minimum level of tacrolimus (cut-off value: 4.6 ng/mL) after transplantation was associated with the production of de novo anti-HLA antibodies. Two other studies identified tacrolimus trough levels associated with HLA antibody production in different types of organ transplantation. Kaneku et al [36] reported that tacrolimus trough levels <3 ng/mL could be associated with de novo anti-HLA antibodies after liver transplantation. Furthermore, tacrolimus trough levels lower than 3.2 ng/mL after kidney transplantation were found to be linked with de novo anti-HLA antibody presence in a center for kidney disease and transplantation in Japan [37]. Despite health improvements in patients with chronic kidney disease, there are many complex immune aspects that still remain to be solved, such as de novo anti-HLA antibodies and immunosuppressive treatment adverse effects [38].
Five years after kidney transplantation, our patients with de novo anti-HLA antibodies had significantly lower long-term death-censored graft survival than those without HLA antibodies (
In the present study, between patient groups, there was a significant difference between survival distributions 5 years after kidney transplantation (
There are also many factors that can affect the outcomes of kidney transplantation. One such factor is donor age: older age of the donor can adversely affect immediate graft function and long-term outcomes [46]. In our study, age was not linked with HLA antibody production, probably because recipients over 65 years of age are still uncommon in Romania, but age was associated with graft loss 5 years after kidney transplantation. Cadaveric donor was another independent factor of the graft loss 5 years after kidney transplantation. Increased recipient age (older than 65 years) or cadaveric donors were also identified as independent risk factors for the development of chronic renal allograft failure in White patients [46,47]. In contrast, age had no effect on 5-year graft survival in a cohort of 627 kidney transplant patients [48].
The immune system has developed strategies for determining whether cells are “self” or “non-self” (foreign) by evaluating HLA genes which are extremely polymorphic and differ from one individual to another [36].
HLA proteins play key roles in immune function, including antigen presentation proteins or complement system components [49]. For successful kidney transplantation, HLA markers must be matched between the organ donor and recipient [50].
When the immune system detects foreign antigens, a series of processes involving T cells and B cells occur that can lead to anti HLA antibodies production [51]. The appearance of HLA alloantibodies is attributed to the exposure of the recipient’s immune system to foreign HLA molecules in multiple pregnancies, transfusions, or previous transplants. Antibody responses begin with the activation of B cells, with specific immunoglobulin-like surface receptors that bind to epitopes on immunizing antigens [52]. Their interactions with helper T cells result in proliferation, affinity maturation, and immunoglobulin class switching, and eventually, differentiation into antibody-producing plasma cells [53]. The immunogenetic relationship between the antibody producer and the immunizing allele affects the antibody response to a mismatched epitope [54]. Previous research has revealed that antibodies to HLA are linked to poor kidney transplant outcomes [55,56]. However, this does not fully explain why some patients have a functional graft even after 5 years, while others, transplanted under the same conditions, reject the graft. Many transplant centers use desensitization methods, such as plasmapheresis, intravenous immunoglobulin, and bortezomib, to remove anti-HLA antibodies [57], but these efforts have often had limited success and are expensive.
The major limitations of our study were the small number of patients and the short follow-up time. As a result, changes in transplant procedures and immunosuppression over time may have led to an overestimation of survival in our study [58]. Other limitations are represented by the kits used to analyze the anti-HLA antibodies that are suitable for identifying the target protein but lack the possibility of quantifying the antibody levels and the mean fluorescence intensity cut-off value, which may differ from values used in other laboratories. However, this is the first report of the association between immunosuppressive therapy and the production of de novo anti-HLA antibodies after transplantation and graft survival in the Romanian population.
Future studies should address the above-mentioned limitations to determine if increasing the number of patients and follow-up time will confirm our findings.
Conclusions
This study showed that anti-HLA antibodies 5 years after kidney transplantation were significantly associated with graft failure. The findings support previous studies and indicate that monitoring of anti-HLA antibodies should be considered in patients undergoing renal transplantation.
Figures
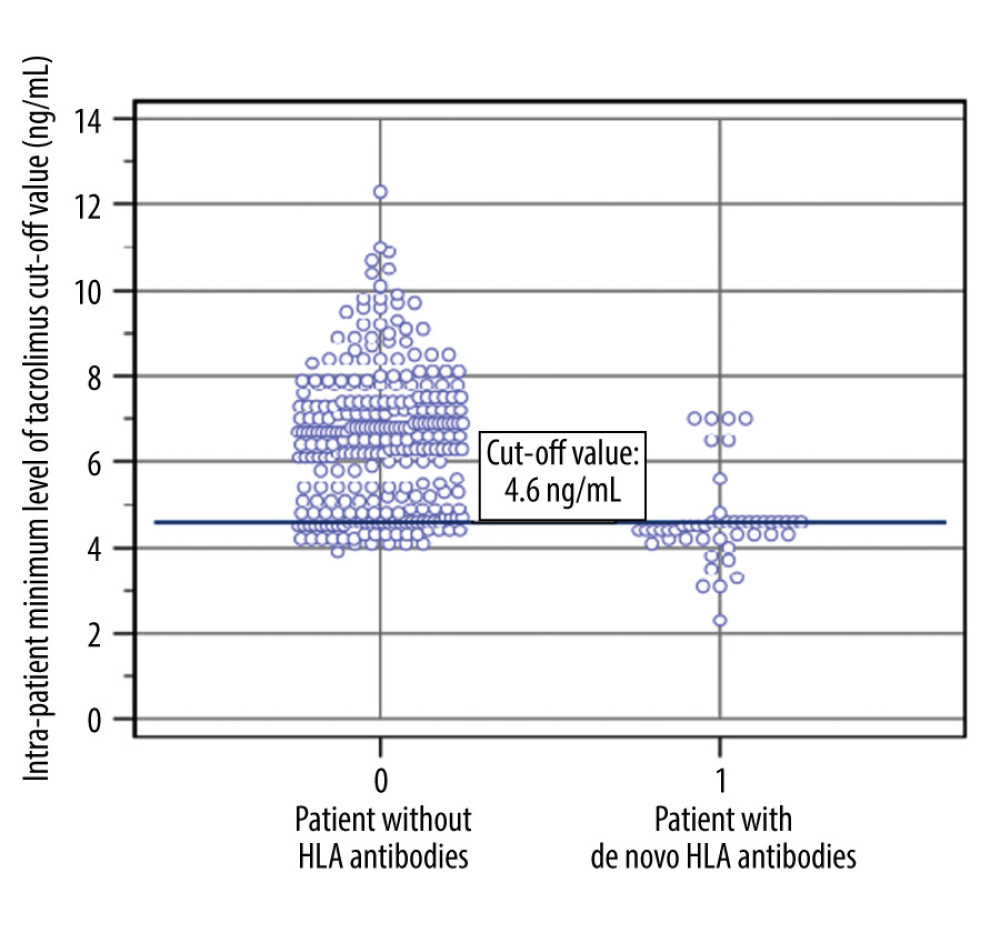 Figure 1. Cut-off value for the appearance of de novo human leucocyte antigen (HLA) antibodies.
Figure 1. Cut-off value for the appearance of de novo human leucocyte antigen (HLA) antibodies. 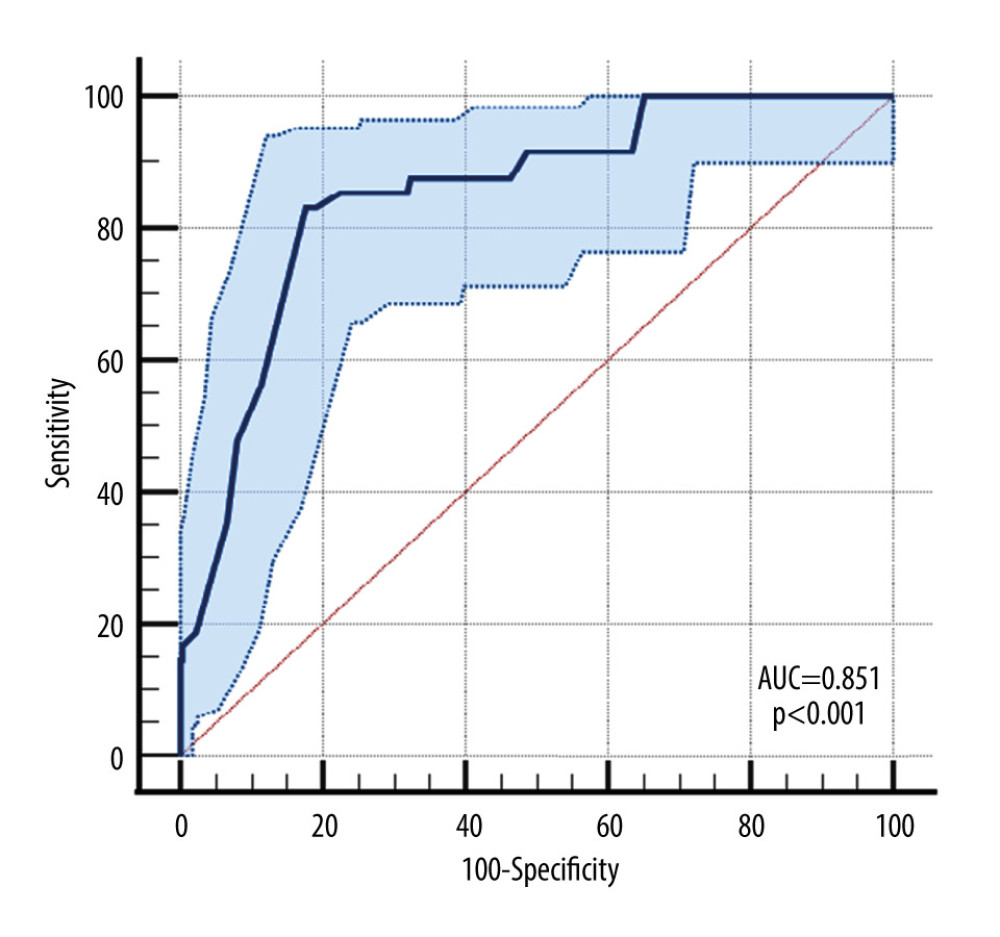 Figure 2. Area under curve (AUC). Because P value is less than 0.05, the area under the receiver operating characteristic (ROC) curve is substantially different from 0.5, implying that the laboratory test has the capacity to identify patients at risk to develop human leucocyte antigen (HLA) antibodies.
Figure 2. Area under curve (AUC). Because P value is less than 0.05, the area under the receiver operating characteristic (ROC) curve is substantially different from 0.5, implying that the laboratory test has the capacity to identify patients at risk to develop human leucocyte antigen (HLA) antibodies. 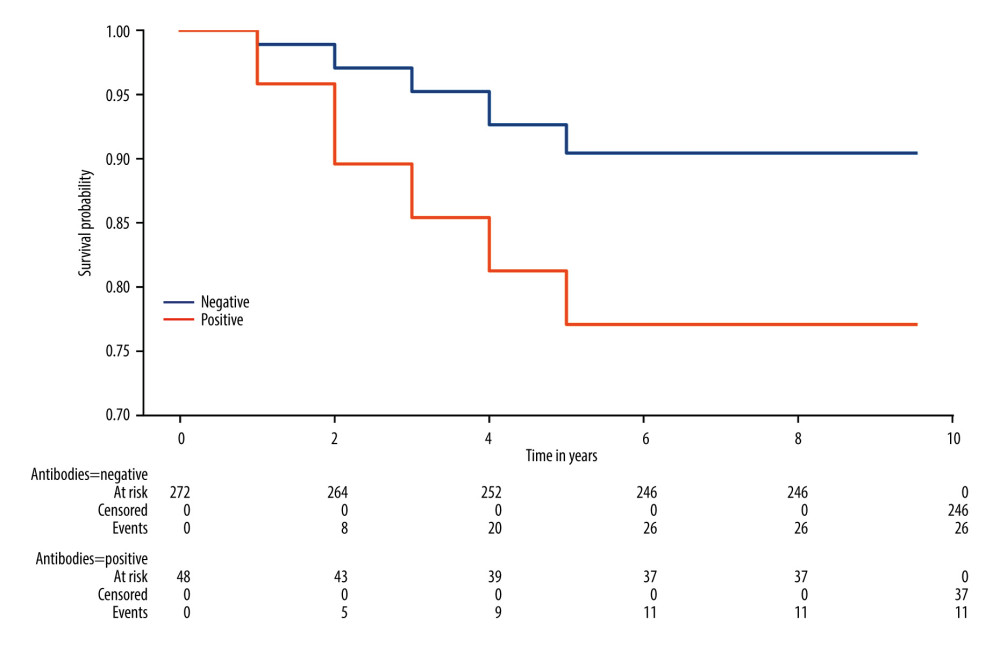 Figure 3. The survival graft rates in patients without preformed anti-human leucocyte antigen (HLA) antibodies.
Figure 3. The survival graft rates in patients without preformed anti-human leucocyte antigen (HLA) antibodies. 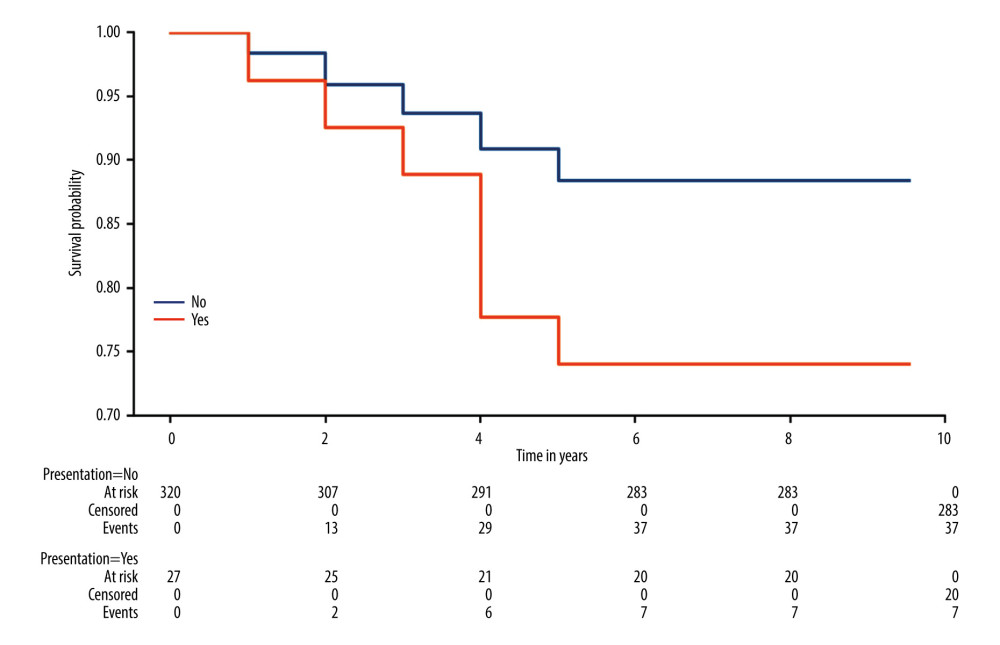 Figure 4. _Survivals rate according to status of human leucocyte antigen (HLA) immunization before kidney transplantation.
Figure 4. _Survivals rate according to status of human leucocyte antigen (HLA) immunization before kidney transplantation. Tables
Table 1. Characteristics of patients with a kidney transplant.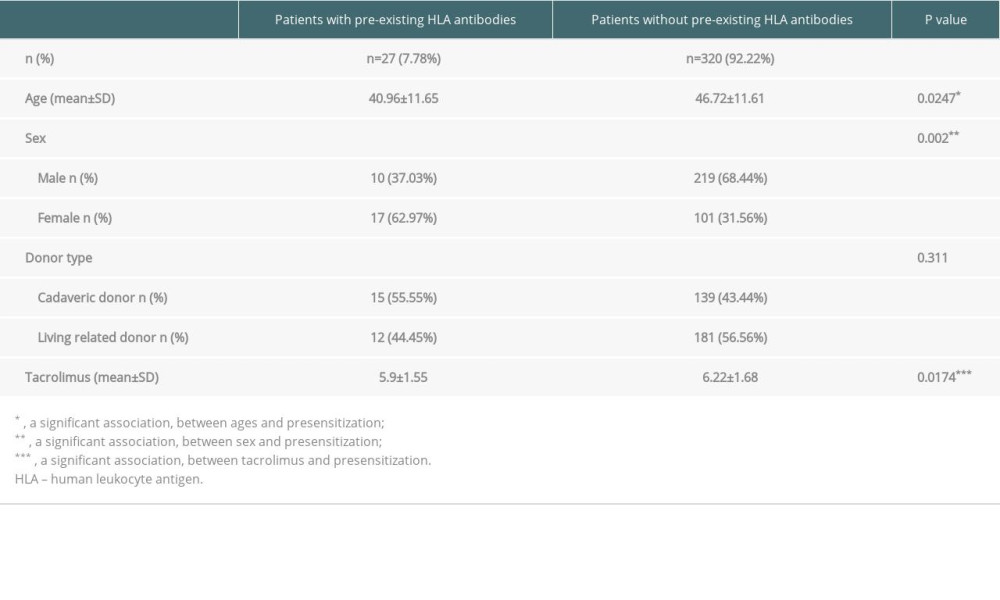 Table 2. Prevalence of posttransplant de novo HLA antibodies.
Table 2. Prevalence of posttransplant de novo HLA antibodies.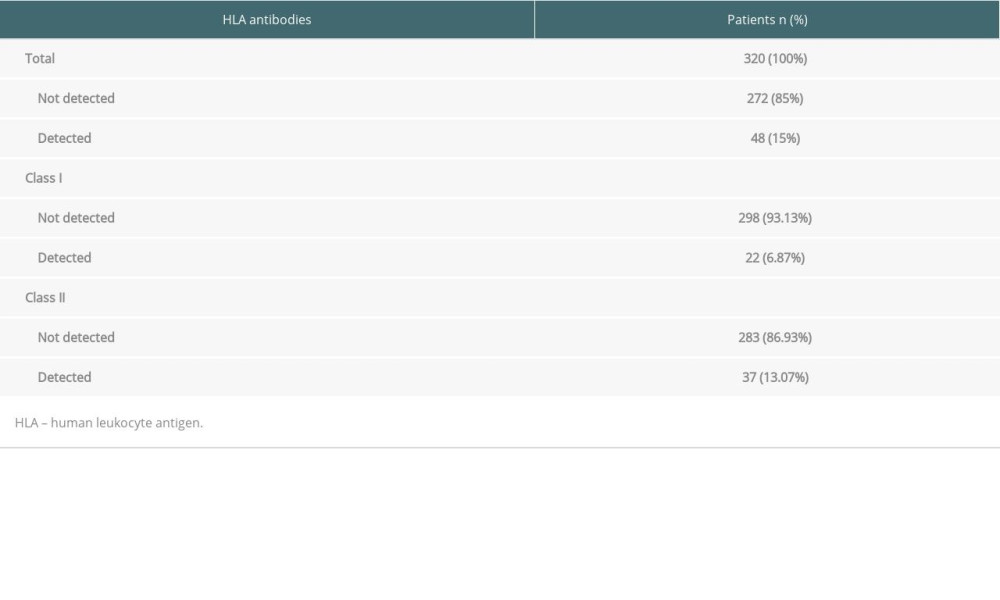 Table 3. Outcome in patients with or without de novo HLA antibodies.
Table 3. Outcome in patients with or without de novo HLA antibodies.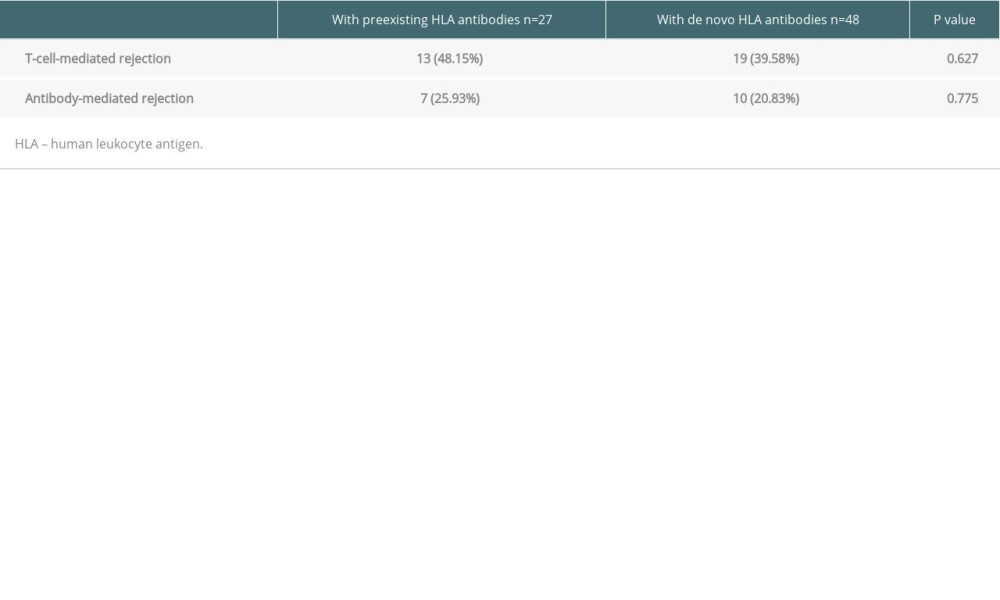 Table 4. Graft survival rates in patients without preexisting anti-HLA antibodies.
Table 4. Graft survival rates in patients without preexisting anti-HLA antibodies.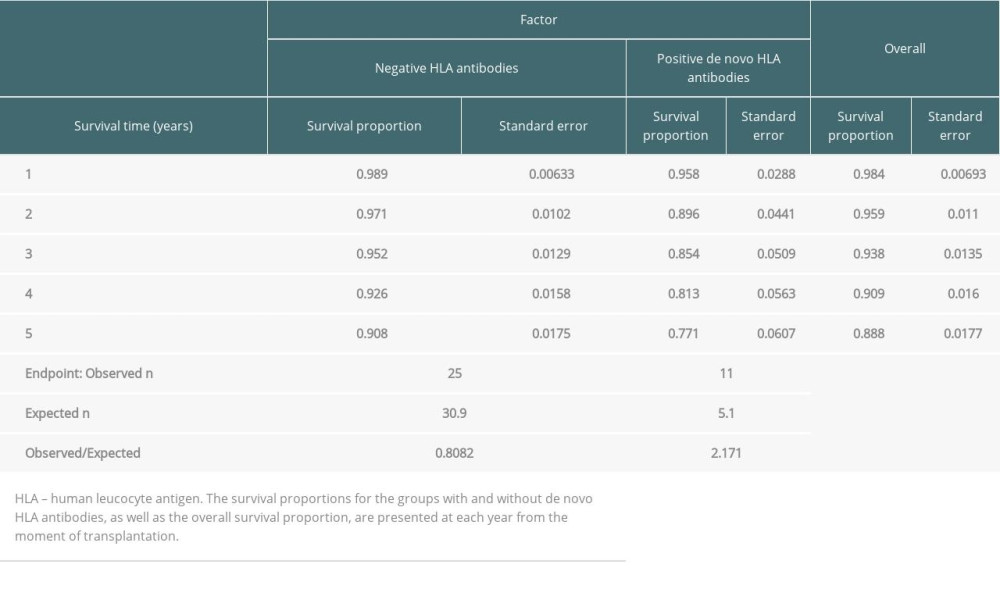 Table 5. Comparison of survival curves (log-rank test).
Table 5. Comparison of survival curves (log-rank test).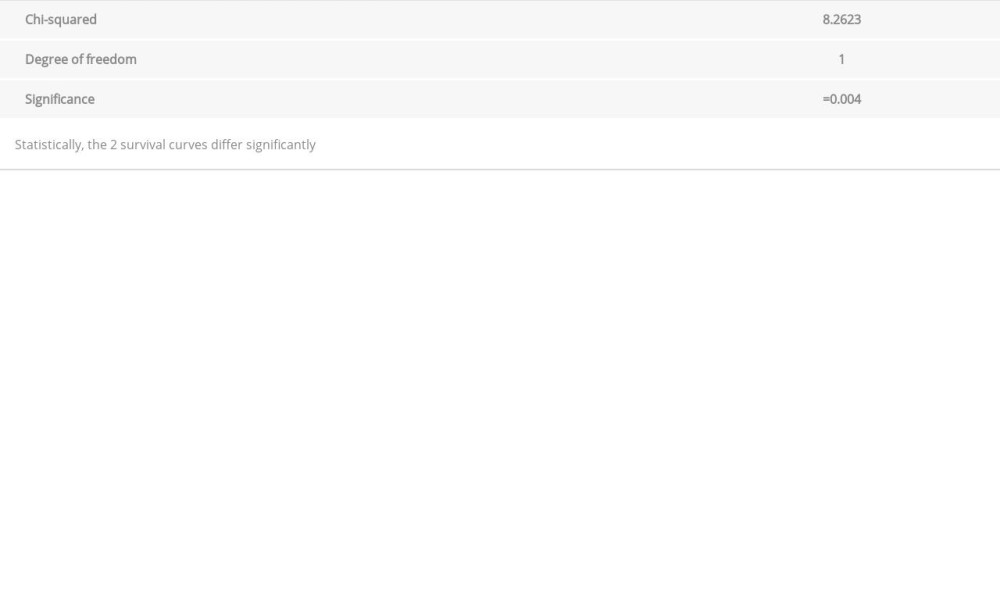 Table 6. Hazard ratios with 95% confidence interval in patients without preformed anti-HLA antibodies.
Table 6. Hazard ratios with 95% confidence interval in patients without preformed anti-HLA antibodies.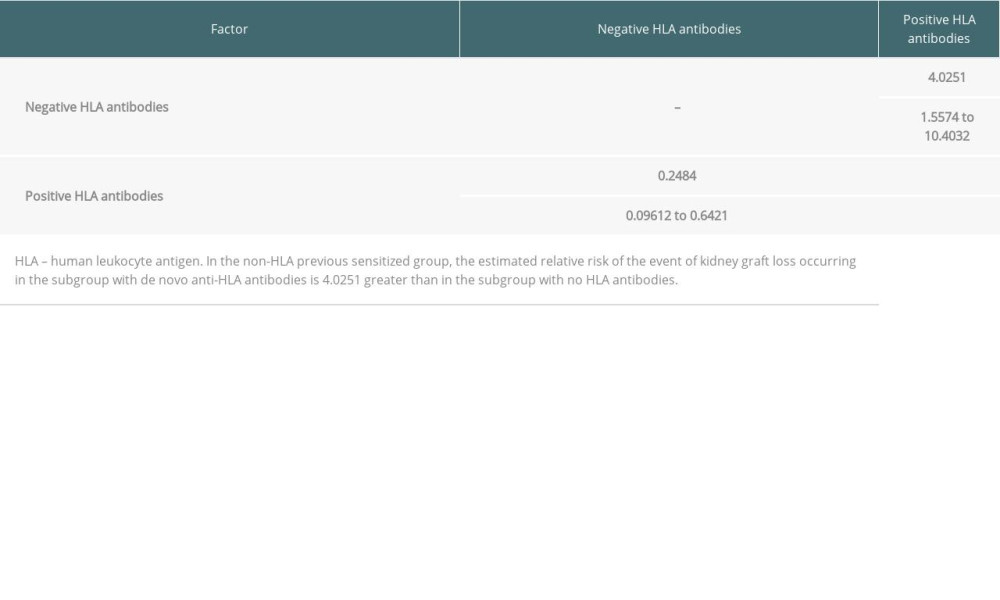
References
1. Muduma G, Shupo FC, Dam S, Patient survey to identify reasons for non-adherence and elicitation of quality of life concepts associated with immunosuppressant therapy in kidney transplant recipients: Patient Prefer Adherence, 2016; 10; 27-36
2. Orandi BJ, Luo X, Massie AB, Survival benefit with kidney transplants from HLA-incompatible live donors: N Engl J Med, 2016; 374(10); 940-50
3. Krishnan N, Abimbola A, Machan N, HLA antibody incompatible renal transplantation: Long-term outcomes similar to deceased donor transplantation: Transplant Direct, 2021; 7(8); e732
4. Alelign T, Ahmed MM, Bobosha K, Kidney transplantation: The challenge of human leukocyte antigen and its therapeutic strategies: J Immunol Res, 2018; 2018; 5986740
5. Claeys E, Vermeire K, Immunosuppressive drugs in organ transplantation to prevent allograft rejection: Mode of action and side effects: J Immunol Sci, 2019; 3(4); 14-21
6. Kalluri HV, Hardinger KL, Current state of renal transplant immunosuppression: Present and future: World J Transplant, 2012; 2(4); 51-68
7. Zhang R, Donor-specific antibodies in kidney transplant recipients: Clin J Am Soc Nephrol, 2018; 13(1); 182-92
8. de Sousa MV, Gonçalez AC, Zollner RL, Mazzali M, Effect of preformed or de novo anti-HLA antibodies on function and graft survival in kidney transplant recipients: Ann Transplant, 2018; 23; 457-66
9. Zecher D, Bach C, Staudner C, Böger CA, Characteristics of donor-specific anti-HLA antibodies and outcome in renal transplant patients treated with a standardized induction regimen: Nephrol Dial Transplant, 2017; 32(4); 730-37
10. Phillpott M, Daga S, Higgins R, Dynamic behaviour of donor specific antibodies in the early period following HLA incompatible kidney transplantation: Transpl Int, 2022; 35; 10128
11. Yamada C, Ramon DS, Cascalho M, Efficacy of plasmapheresis on donor-specific antibody reduction by HLA specificity in post-kidney transplant recipients: Transfusion, 2015; 55(4); 727-35 quiz 726
12. Casan JML, Wong J, Northcott MJ, Opat S, Anti-CD20 monoclonal antibodies: Reviewing a revolution: Hum Vaccin Immunother, 2018; 14(12); 2820-41
13. Althaf MM, El Kossi M, Jin JK, Sharma A, Halawa AM, Human leukocyte antigen typing and crossmatch: A comprehensive review: World J Transplant, 2017; 7(6); 339-48
14. Peacock S, Briggs D, Barnardo M, BSHI/BTS guidance on crossmatching before deceased donor kidney transplantation: Int J Immunogenet, 2022; 49(1); 22-29
15. William RM, Fiona H, Darren L, Tissue typing, crossmatching and the allocation of deceased donor kidney transplants: Transplantation Surgery, 2021; 31-50, New York, Springer
16. Jamshidian Tehrani N, Geramizadeh B, Malekhosseini SA, Virtual crossmatching in kidney transplantation, Shiraz experience in development of a web-based program: Int J Organ Transplant Med, 2021; 12(2); 20-25
17. Faresjö M, A useful guide for analysis of immune mediators in cancer by fluorochrome (Luminex) technique: Methods Mol Biol, 2020; 2108; 3-13
18. Colombo MB, Haworth SE, Poli F, Luminex technology for anti-HLA antibody screening: evaluation of performance and of impact on laboratory routine: Cytometry B Clin Cytom, 2007; 72(6); 465-71
19. Pandey P, Pande A, Mishra S, Significance of Luminex-crossmatch assay and its mean fluorescence intensity – a retrospective observation in 380 renal transplant cases: Pol Przegl Chir, 2022; 94(2); 38-48
20. Lachmann N, Todorova K, Schulze H, Schönemann C: Transfus Med Hemother, 2013; 40(3); 182-89
21. Glushakova LG, Alto BW, Kim MS, Multiplexed kit based on Luminex technology and achievements in synthetic biology discriminates Zika, chikungunya, and dengue viruses in mosquitoes: BMC Infect Dis, 2019; 19(1); 418
22. Tang H, Panemangalore R, Yarde M, 384-well multiplexed luminex cytokine assays for lead optimization: J Biomol Screen, 2016; 21(6); 548-55
23. Kupcova SH, Vodickova KK, Vodicka P, Luminex xMAP assay to quantify cytokines in cancer patient serum: Methods Mol Biol, 2020; 2108; 65-88
24. Halloran PF, Reeve JP, Pereira AB, Antibody-mediated rejection, T cell-mediated rejection, and the injury-repair response: new insights from the Genome Canada studies of kidney transplant biopsies: Kidney Int, 2014; 85(2); 258-64
25. Tait BD, Detection of HLA antibodies in organ transplant recipients – triumphs and challenges of the solid phase bead assay: Front Immunol, 2016; 7; 570
26. Roufosse C, Simmonds N, Clahsen-Van Groningen M, A 2018 reference guide to the banff classification of renal allograft pathology: Transplantation, 2018; 102; 1795-814
27. Mo H, Kim SY, Min S, Association of intrapatient variability of tacrolimus concentration with early deterioration of chronic histologic lesions in kidney transplantation: Transplant Direct, 2019; 5(6); e455
28. Terasaki PI, Ozawa M, Predicting kidney graft failure by HLA antibodies: A prospective trial: Am J Transplant, 2004; 4; 438-43
29. O’Leary JG, Samaniego M, Barrio MC, The influence of immunosuppressive agents on the risk of de novo donor-specific. HLA antibody production in solid organ transplant recipients: Transplantation, 2016; 100; 39-53
30. Rodrigo E, Segundo DS, Fernandez-Fresnedo G, Within-patient variability in tacrolimus blood levels predicts kidney graft loss and donor-specific antibody development: Transplantation, 2016; 100; 2479-85
31. Solomon S, Colovai A, Del Rio M, Tacrolimus variability is associated with de novo donor-specific antibody development in paediatric renal transplant recipients: Pediatr Nephrol, 2020; 35; 261-70
32. Park Y, Lee H, Eum SH, Intrapatient variability in tacrolimus trough levels over two years affects the long-term allograft outcomes of kidney transplantation: Front Immunol, 2021; 12; 746013
33. Shuker N, van Gelder T, Hesselink DA, Intra-patient variability in tacrolimus exposure: Causes and consequences for clinical management: Transplant Rev (Orlando), 2015; 29; 78-84
34. Gonzales HM, McGillicuddy JW, Rohan V, A comprehensive review of the impact of tacrolimus intrapatient variability on clinical outcomes in kidney transplantation: Am J Transplant, 2020; 20; 1969-83
35. Kuypers DRJ, Intrapatient variability of tacrolimus exposure in solid organ transplantation: A novel marker for clinical outcome: Clin Pharmacol Ther, 2020; 107; 347-58
36. Kaneku H, O’Leary JG, Banuelos N, De novo donor-specific HLA antibodies decrease patient and graft survival in liver transplant recipients: Am J Transplant, 2013; 13; 5411548
37. Fujiyama N, Satoh S, Saito M, Association of immunosuppressive agents and cytomegalovirus infection with de novo donor-specific antibody development within 1 year after renal transplantation: Int Immunopharmacol, 2019; 76; 105881
38. Claeys E, Vermeire K, Immunosuppressive drugs in organ transplantation to prevent allograft rejection: Mode of action and side effects: J Immunol Sci, 2019; 3(4); 14-21
39. Katerinis I, Hadaya K, Duquesnoy R, De novo anti-HLA antibody after pandemic H1N1 and seasonal influenza immunisation in kidney transplant recipients: Am J Transplant, 2011; 11; 1727-33
40. Mittal S, Page SL, Friend PJ, De Novo donor-specific HLA antibodies: Biomarkers of pancreatic transplant failure: Am J Transplant, 2014; 14; 1664-71
41. Terasaki PI, Ozawa M, Castro R, Four-year follow-up of a prospective trial of HLA and MICA antibodies on kidney graft survival: Am J Transplant, 2007; 7; 408-15
42. Morath C, Opelz G, Zeier M, Süsal C, Clinical relevance of HLA antibody monitoring after kidney transplantation: J Immunol Res, 2014; 2014; 845040
43. Li B, Cairns J, Robb M, Predicting patient survival after deceased donor kidney transplantation using flexible parametric modelling: BMC Nephrol, 2016; 17; 51
44. NHS Blood and Transplant: Organ donation and transplantation activity report 2019/20, 2020 [cited 2021 November]. Available from: https://nhsbtdbe.blob.core.windows.net/umbraco-assets-corp/19220/activity-report-2019-2020.pdf
45. Crux NB, Elahi S, Human leukocyte antigen (HLA) and immune regulation: How do classical and non-classical HLA alleles modulate immune response to human immunodeficiency virus and hepatitis C virus infections?: Front Immunol, 2017; 8; 832
46. Helfer MS, Pompeo JC, Costa ORS, Long-term effects of delayed graft function duration on function and survival of deceased donor kidney transplants: J Bras Nefrol, 2019; 41; 231-41
47. Oweira H, Ramouz A, Ghamarnejad O, Risk factors of rejection in renal transplant recipients: A narrative review: J Clin Med, 2022; 11(5); 1392
48. Fabrizii V, Winkelmayer WC, Klauser R, Patient and graft survival in older kidney transplant recipients: does age matter?: J Am Soc Nephrol, 2004; 15(4); 1052-60
49. Chaplin DD, Overview of the immune response: J Allergy Clin Immunol, 2010; 125; S3-23
50. Kim JJ, Fuggle SV, Marks SD, Does HLA matching matter in the modern era of renal transplantation?: Pediatr Nephrol, 2021; 36(1); 31-40
51. Rees L, Kim JJ, HLA sensitisation: Can it be prevented?: Pediatr Nephrol, 2015; 30; 577-87
52. Gagliani N, Huber S, Basic aspects of T helper cell differentiation: Methods Mol Biol, 2017; 1514; 19-30
53. Garcês S, Demengeot J, The immunogenicity of biologic therapies: Curr Probl Dermatol, 2018; 53; 37-48
54. Eng HS, Bennett G, Bardy P, Coghlan P, Clinical significance of anti-HLA antibodies detected by Luminex: enhancing the interpretation of CDC-BXM and important post-transplantation monitoring tools: Hum Immunol, 2009; 70; 595-99
55. Hassan S, Regan F, Brown C, Shared alloimmune responses against blood and transplant donors result in adverse clinical outcomes following blood transfusion post-renal transplantation: Am J Transplant, 2019; 19; 1720-29
56. Cherukuri A, Mehta R, Sharma A, Post-transplant donor specific antibody is associated with poor kidney transplant outcomes only when combined with both T-cell-mediated rejection and non-adherence: Kidney Int, 2019; 96(1); 202-13
57. Boonyaratanakornkit J, Taylor JJ, Techniques to study antigen-specific B cell responses: Front Immunol, 2019; 10; 1694
58. Graham CN, Watson C, Barlev A, Mean lifetime survival estimates following solid organ transplantation in the US and UK: J Med Econ, 2022; 25(1); 230-37
Figures
 Figure 1. Cut-off value for the appearance of de novo human leucocyte antigen (HLA) antibodies.
Figure 1. Cut-off value for the appearance of de novo human leucocyte antigen (HLA) antibodies. Figure 2. Area under curve (AUC). Because P value is less than 0.05, the area under the receiver operating characteristic (ROC) curve is substantially different from 0.5, implying that the laboratory test has the capacity to identify patients at risk to develop human leucocyte antigen (HLA) antibodies.
Figure 2. Area under curve (AUC). Because P value is less than 0.05, the area under the receiver operating characteristic (ROC) curve is substantially different from 0.5, implying that the laboratory test has the capacity to identify patients at risk to develop human leucocyte antigen (HLA) antibodies. Figure 3. The survival graft rates in patients without preformed anti-human leucocyte antigen (HLA) antibodies.
Figure 3. The survival graft rates in patients without preformed anti-human leucocyte antigen (HLA) antibodies. Figure 4. _Survivals rate according to status of human leucocyte antigen (HLA) immunization before kidney transplantation.
Figure 4. _Survivals rate according to status of human leucocyte antigen (HLA) immunization before kidney transplantation. Tables
 Table 1. Characteristics of patients with a kidney transplant.
Table 1. Characteristics of patients with a kidney transplant. Table 2. Prevalence of posttransplant de novo HLA antibodies.
Table 2. Prevalence of posttransplant de novo HLA antibodies. Table 3. Outcome in patients with or without de novo HLA antibodies.
Table 3. Outcome in patients with or without de novo HLA antibodies. Table 4. Graft survival rates in patients without preexisting anti-HLA antibodies.
Table 4. Graft survival rates in patients without preexisting anti-HLA antibodies. Table 5. Comparison of survival curves (log-rank test).
Table 5. Comparison of survival curves (log-rank test). Table 6. Hazard ratios with 95% confidence interval in patients without preformed anti-HLA antibodies.
Table 6. Hazard ratios with 95% confidence interval in patients without preformed anti-HLA antibodies. Table 1. Characteristics of patients with a kidney transplant.
Table 1. Characteristics of patients with a kidney transplant. Table 2. Prevalence of posttransplant de novo HLA antibodies.
Table 2. Prevalence of posttransplant de novo HLA antibodies. Table 3. Outcome in patients with or without de novo HLA antibodies.
Table 3. Outcome in patients with or without de novo HLA antibodies. Table 4. Graft survival rates in patients without preexisting anti-HLA antibodies.
Table 4. Graft survival rates in patients without preexisting anti-HLA antibodies. Table 5. Comparison of survival curves (log-rank test).
Table 5. Comparison of survival curves (log-rank test). Table 6. Hazard ratios with 95% confidence interval in patients without preformed anti-HLA antibodies.
Table 6. Hazard ratios with 95% confidence interval in patients without preformed anti-HLA antibodies. In Press
Original article
Diagnostic Utility of FAR1 Methylation Levels in Hepatocellular Carcinoma Patients Undergoing Liver Transpl...Ann Transplant In Press; DOI: 10.12659/AOT.951568
Original article
Inferior Long-Term Outcome of Fatty Liver Allografts After Orthotopic Liver TransplantationAnn Transplant In Press; DOI: 10.12659/AOT.950589
Database Analysis
Identification and Validation of Liver Transplantation-Induced Acute Lung Injury Biomarkers Using a Bioinfo...Ann Transplant In Press; DOI: 10.12659/AOT.950289
Original article
Survival and Recurrence in Liver Transplant Patients With Intrahepatic Cholangiocarcinoma and Hepatocellula...Ann Transplant In Press; DOI: 10.12659/AOT.950997
Most Viewed Current Articles
24 Aug 2021 : Review article 18,372
Normothermic Machine Perfusion (NMP) of the Liver – Current Status and Future PerspectivesDOI :10.12659/AOT.931664
Ann Transplant 2021; 26:e931664
05 Apr 2022 : Original article 14,731
Impact of Statins on Hepatocellular Carcinoma Recurrence After Living-Donor Liver TransplantationDOI :10.12659/AOT.935604
Ann Transplant 2022; 27:e935604
22 Nov 2022 : Original article 14,244
Long-Term Effects of Everolimus-Facilitated Tacrolimus Reduction in Living-Donor Liver Transplant Recipient...DOI :10.12659/AOT.937988
Ann Transplant 2022; 27:e937988
29 Dec 2021 : Original article 13,752
Efficacy and Safety of Tacrolimus-Based Maintenance Regimens in De Novo Kidney Transplant Recipients: A Sys...DOI :10.12659/AOT.933588
Ann Transplant 2021; 26:e933588








