19 July 2022: Original Paper
Graft Inflow Modulation in Living-Donor Liver Transplantation: Hepatic Hemodynamic Changes in Splenic Artery Ligation and Splenectomy
Che-Min Su1ABCDEF, Tsung-Ching Chou1ABD, Tsung-Han Yang1ABD, Yih-Jyh Lin1ABDEF*DOI: 10.12659/AOT.936609
Ann Transplant 2022; 27:e936609
Abstract
BACKGROUND: Excessive portal flow to an allograft was a key mechanism for small-for-size syndrome in living-donor liver transplantation (LDLT). Good outcomes in LDLT by graft inflow modulation (GIM) using a small graft were reported, but the effect on hepatic hemodynamics is undefined. This report summarizes our experience with GIM and compares the effects of splenic artery ligation (SAL) and splenectomy on hepatic hemodynamic changes.
MATERIAL AND METHODS: Ninety-nine patients who underwent adult-to-adult LDLT from June 2014 to December 2020 were included in this study. GIM was performed in 36 patients (17 patients with SAL and 19 with splenectomy).
RESULTS: The GIM group had lower graft-to-recipient weight compared to the no-modulation group (median, 0.91% versus 1.04%, P=0.022). Initial portal venous flow (PVF) was higher in the GIM group (median, 311 versus 156 ml/min/100 g, P<0.001). After GIM, PVF decreased to 224 ml/min/100 g. One-year graft survival with GIM was 89.9%, and for the no-modulation group it was 86.6% (P=0.945). In the subgroup analysis, the efficacy of decompressing PVF was higher in the splenectomy subgroup (median, 14.3% versus 41.8%, P=0.002).
CONCLUSIONS: GIM was useful for grafts with high PVF. Splenectomy modulated excessive PVF more effectively than did SAL. Perioperative hepatic hemodynamic changes could assist surgeons in selecting different GIM strategies.
Keywords: Hypertension, Portal, Liver Transplantation, Splenectomy, Adult, Hemodynamics, Hepatic Artery, Humans, Liver, Living Donors, Portal Vein, Splenic Artery
Background
Living-donor liver transplantation (LDLT) is an established alternative to deceased-donor liver transplantation (DDLT). Initially developed for pediatric recipients, LDLT was successively extended to adult patients with end-stage liver disease, including hepatocellular carcinoma (HCC) [1,2]. Since the introduction of LDLT, donor-recipient size matching has become a concern. Considering donor safety, the recipient may have small-for-size syndrome (SFSS) if the liver graft is too small to meet the recipient’s metabolic demand. SFSS is clinically manifested by impaired coagulation, cholestasis, and ascites, with subsequent septic complications and lower graft survival [3,4]. Excessive portal flow to the allograft was considered a key mechanism resulting in sinusoid congestion and hemorrhage [5]. Several investigators have reported good outcomes in LDLT using a small graft by surgical graft inflow modulation (GIM), including splenic artery ligation (SAL) [6,7], splenectomy [8,9], and portosystemic shunt (PSS) [10,11]. SAL decreased splenic vein flow, with a corresponding increase in hepatic artery (HA) flow. Splenectomy can produce a major reduction in portal venous flow (PVF), comparable to PSS, without the risk of portal steal syndrome. Modulation to keep portal venous pressure (PVP) <15 mmHg [8] or PVF <250 ml/min/100 g graft weight [12] was associated with favorable outcomes. However, the effect on hepatic hemodynamics by different types of surgical GIM in LDLT is not well understood. This study summarizes our experience with GIM and compares the effects of SAL and splenectomy on hepatic hemodynamic changes and clinical outcomes.
Material and Methods
Study Design
STUDY DESIGN:
We retrospectively reviewed the data for patients who underwent adult-to-adult LDLT from June 2014 to December 2020 at the National Cheng Kung University Hospital in Taiwan. Re-transplant patients were excluded. The patients were followed up after surgery until June 2021, death, or the date of the last follow-up visit, whichever came first. The study was approved by our institutional review board (B-ER-110-304).
PREOPERATIVE DONOR EVALUATION:
Indications for LDLT were equivalent to those for DDLT except for patients with HCC. Donors were selected from among candidates who volunteered to be living donors. All potential living donors were evaluated by a multidisciplinary team of transplant surgeons, transplant hepatologists, clinical psychologists, and nurse specialists. Donor computed tomography (CT) was performed for volumetric analysis. Decisions about graft types were based on the preoperatively predicted graft-to-recipient weight ratio (GRWR). In general, GRWR >0.8% was accepted. The donor liver remnant must be >30% of the total donor liver volume. Actual GRWR was calculated by graft weight measured after cold graft perfusion.
SURGERY:
The right lobe liver graft excluding the middle hepatic vein (MHV) was the preferred choice in our center. The MHV tributaries draining the segment 5 vein (V5), the segment 8 vein (V8), and the inferior right hepatic vein were reconstructed when their diameter was >5 mm. In left-lobe grafts, the common orifice of the MHV and left hepatic vein were directly anastomosed to the recipient’s inferior vena cava in a triangular manner.
GRAFT INFLOW MODULATION:
Intraoperative measurement of the portal vein (PV) and HA flow used transit-time flow methods with the Medi-Stim VeriQ™ System (Oslo, Norway). Appropriate size probes (ranging from 4 to 12 mm in diameter) were applied to the HA and PV based on the target vessel diameter. PVP was measured with a 25-G catheter with direct puncture. The measurement timing was performed after PV and HA anastomosis/reperfusion and after flow modulation. The flow modulation indication was as follows: initial PVF >250 ml/min/100 g. GIM was not limited to grafts with a GRWR <0.8. A post-perfusion PVF of 100–250 ml/min/100 g was considered optimal. The preferred method for GIM was SAL. The splenic artery was isolated at the superior border of the pancreas. If portal flow or pressure changes after clamping the splenic artery were unsatisfactory, splenectomy was performed. Ligation of varices or shunting was performed in recipients with insufficient portal flow.
POSTOPERATIVE CARE: The patients were transferred to the intensive care unit after surgery. We performed Doppler ultrasound daily to assess the patency of the HA, PV, and hepatic vein for all recipients within 1 week after the operation. SFSS and early allograft dysfunction (EAD) were defined using criteria previously reported [3,13].
IMMUNOSUPPRESSION:
The immunosuppression protocol was standardized with calcineurin inhibitors (CNIs) (tacrolimus/cyclosporine), mycophenolate mofetil, and steroids. No induction agents were used. Intraoperative methylprednisolone was given except for emergent LDLT. Mammalian target of rapamycin (mTOR) inhibitors (sirolimus/everolimus) were added for patients with HCC at 1 month after the operation. After splenectomy, vaccination against streptococcus pneumonia was provided 1 year after LDLT.
STATISTICAL ANALYSIS:
Continuous parameters are presented as the median and interquartile range (IQR). Categorical variables are expressed as frequency and percentage. The Pearson chi-squared test for categorical variables and the Mann-Whitney U test/Wilcoxon signed-rank test for continuous variables were used to compare groups.
Graft survival was measured from the time of transplantation to death from any cause or re-transplantation. The Kaplan-Meier method was used to analyze survival, and the log-rank test was used for comparisons. Statistical significance was defined as a
Results
PVF and PVP
PVF AND PVP:
Initial PVF (after reperfusion) was significantly higher in the GIM group than in the no-modulation group (median, 311 versus 156 ml/min/100 g, P<0.001, Table 2). After modulation, PVF decreased to 224 ml/min/100 g and was still higher (P<0.001). Initial hepatic artery flow (HAF) was significantly lower in the GIM group. After modulation, the HAF values were similar between the 2 groups (median, 100 versus 80 ml/min, P=0.065, Table 2).
The final PVP was measured in 47 patients in the no-modulation group, with a median value of 14 mmHg (IQR, 10–17 mmHg). The final portal pressure was measured in the SAL subgroup in 9 patients (median, 14; IQR, 13–15 mmHg). The final portal pressure was measured in 10 patients (median, 11; IQR, 9–14 mmHg) in the splenectomy subgroup. We observed that in the modulation group, there were 17 patients with a final PVP <15 mmHg (19 patients with a record).
SAL VERSUS SPLENECTOMY: In the GIM group, 36 patients were further divided into SAL and splenectomy subgroups. Tables 3 and 4 present a comparison of the clinical and operative characteristics. More female recipients, female donors and older donor age were observed in the splenectomy subgroup. The liver graft was smaller in the splenectomy subgroup. More left-lobe grafts were used. The GRWR (median, 0.99% versus 0.83%, P=0.038) were lower in the splenectomy subgroup compared to the SAL subgroup. The postoperative complications, incidence of SFSS, EAD, hospital stays, blood losses, and operative times were similar between the 2 subgroups.
In the SAL subgroup, the median value of PVF decreased from 292 to 233 ml/min/100 g (P<0.001) and the median value of HAF increased from 70 to 83 ml/min (P<0.01). In the splenectomy subgroup, the median value of PVF decreased from 319 to 203 ml/min/100 g (P<0.001) and the median value of HAF increased from 40 to 73 ml/min (P<0.01). The efficacy of decompressing PVF was higher in the splenectomy subgroup than in the SAL subgroup (median, 14.3% versus 41.8%, P=0.002, Table 4). The increase in HAF was also higher in the splenectomy subgroup.
SPLENECTOMY-RELATED COMPLICATIONS:
Five (8.3%) patients had splenectomy-related complications. Pancreatic pseudocyst formation developed in 1 recipient and CT-guided drainage was performed. Pancreatic fistula was treated by prolonged drainage in 1 recipient. The other patient developed retroperitoneal hematoma and received conservative treatment. Two patients developed portal vein thrombosis after splenectomy. One patient was treated with anticoagulants successfully, and the other patient developed portal vein thrombosis on postoperative day 1 and received re-transplantation 3 days later. The cause of portal vein thrombosis in the re-transplant patient might have been due to portal vein compression because of the poor position of left-lobe graft. In addition, a huge spleen with IMV directly joining into SMV might be considered a predisposing factor. No SAL-related complications were noted.
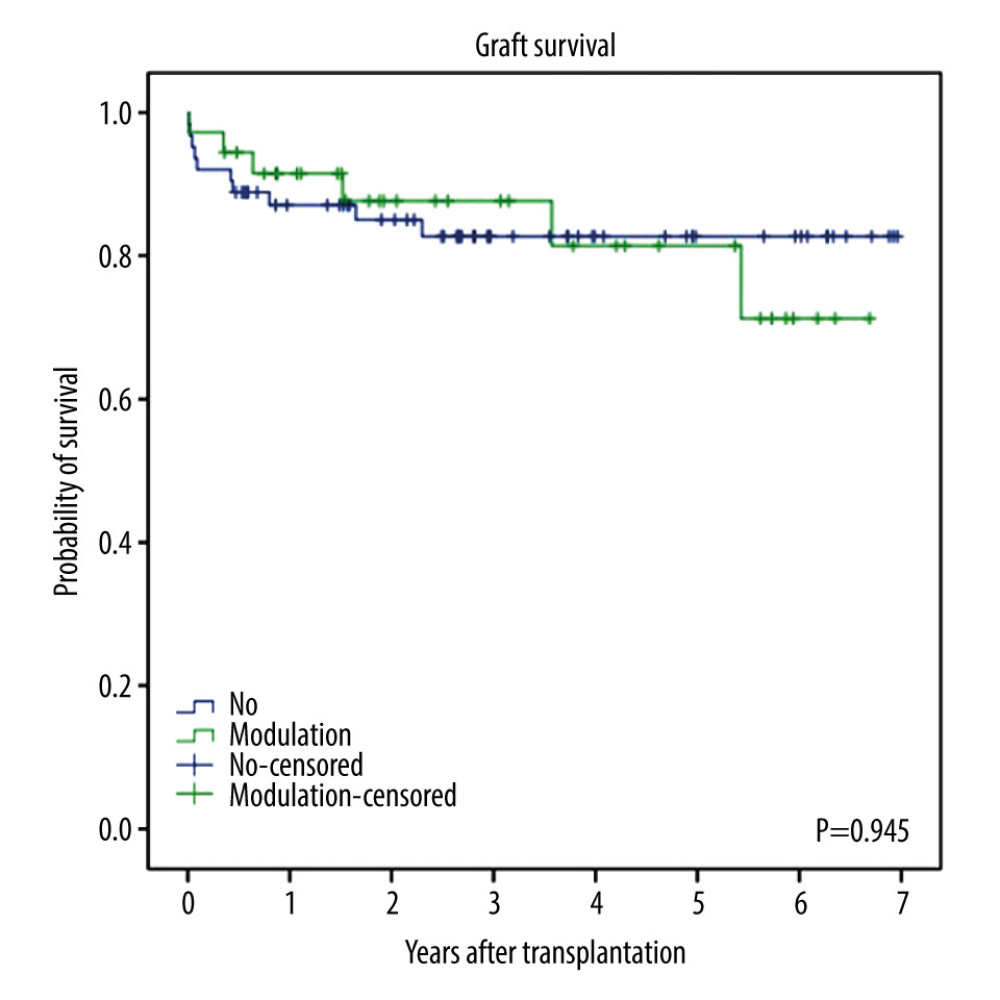
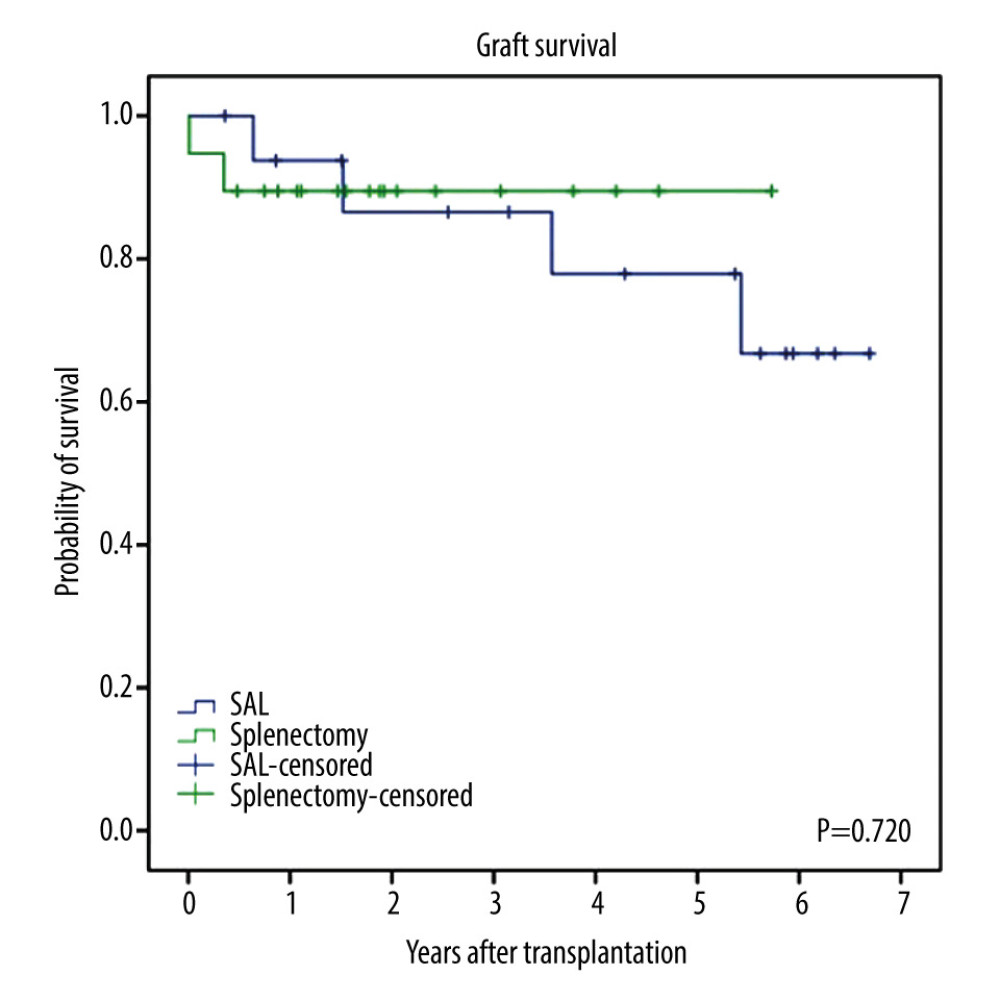
GRAFT SURVIVAL: Figure 1 shows graft survival according to use of modulation. The 1-year graft survival for patients with modulation was 89.9% and was comparable to that in the no-modulation group (86.6%, P=0.945). Figure 2 shows graft survival according to modulation type. The 1-year graft survival was 90.8% for patients with SAL and 89.3% for splenectomy, but the difference was not significant (P=0.720).
Discussion
A donor liver is considered a small-for-size graft when the GRWR is <0.8 or when the ratio between the graft volume to standard liver volume is <40% [14]. High portal flow and pressure are detrimental for small-for-size grafts, leading to sinusoidal congestion, ischemic microcirculation, and subsequent graft failure [15]. During the intraoperative period, surgical GIM could reduce PVF and PVP. The most appropriate hemodynamic parameter in determining the utilization of GIM remains a subject of discussion. Ogura et al [8], in a retrospective analysis, reported that a PVP <15 mmHg was associated with good patient outcomes. Kaido et al reported improved outcomes in smaller grafts in whom the pressure could be lowered to <15 mmHg [16]. A cut-off of 250 ml/min/100 g of liver grafts was previously proposed by 2 studies [10,12]. In our study, we measured PVP and PVF simultaneously. However, we found that PVP was influenced by central venous pressure (CVP). Sainz-Barriga et al also reported that increases in the CVP were transmitted to the PVP. The evaluation of PHT severity with PVP could be misleading [17]. Therefore, we used PVF as a GIM indicator because PVF measurement was not only helpful in portal hyperperfusion state, but also avoided portal hypoperfusion. In addition, we measured PVF and HAF together to ensure adequate hepatic artery flow.
SFSS is a multifactorial phenomenon. Besides graft size, other risk factors for SFSS should be considered. Graft steatosis [18], hepatic arterial flow [19], hepatic venous outflow [20], cold ischemic time, and recipient factors (portal hypertension, MELD score) have been reported [21,22]. Thus, we had a relatively liberal indication for GIM, not only limited to grafts with a GRWR <0.8%. We think that maintaining an optimal PVF for grafts with some risk factors for SFSS is important.
Our study demonstrated that PVF could be successfully decreased to within the normal range in the GIM group. Despite the use of the smaller graft, by the aid of GIM, the incidence of SFSS and early graft survival were not inferior to those in the no-modulation group. Some studies have shown the benefit of GIM in LDLT by different techniques. A multi-center study reported by Emond et al identified a higher rate of graft dysfunction in modulated subjects; however, graft survival in modulated subjects was no different from in no-modulated subjects at 3 years [23]. In this study, we directly compared hepatic hemodynamic changes between the SAL and splenectomy subgroups in the cohort.
SAL is a simple and effective way to reduce PVF and is an alternative to splenectomy. This finding is mainly based on the principle that the level of spleen-derived perfusion is an important factor in portal inflow [7,9,24]. However, several investigators have reported that SAL is insufficient compared with splenectomy and portosystemic shunt [25,26]. In our study, the preferred method for GIM was SAL. Splenectomy was performed if the effect of portal decompression by SAL was insufficient. We found that SAL decreased portal blood flow by 14.3%. Splenectomy had higher efficacy for decompressing portal flow (41.8%) than SAL. We also found that splenectomy was indicated for smaller liver grafts and the higher PVF group.
A Tokyo group reported that splenectomy was associated with longer operative time, higher blood loss, and higher risk of venous thrombosis and infection [27]. We found that the incidence of venous thrombosis was not higher in the splenectomy subgroup than in the SAL subgroup. No severe bacterial infections were observed. The blood losses and operative times were similar between the splenectomy and the SAL subgroups. Two patients developed portal vein thrombosis after splenectomy.
In contrast, 4 patients had portal vein thrombosis in the no-modulation group. Thus, splenectomy could be considered in patients with high PVF and should have an acceptable complication rate. The Kyushu group recently reported that simultaneous splenectomy is recommended for a small graft or patients with portal hypertension or high portal pressure in adult LDLT recipients [28].
Moon et al reported that splenic devascularization could replace splenectomy, with lesser complications [29]. However, the effect of the procedure requires further clarification. Although PSS was considered an effective method to decrease portal flow [10,11], we did not perform portosystemic shunt routinely because of the risk of portal hypoperfusion and encephalopathy. Pharmacologic manipulation with somatostatin therapy is one method of GIM. Hessheimer et al reported that somatostatin reduced portal vein flow and protected sinusoidal endothelial cells in their model [30]. Recently, Troisi et al found that somatostatin decreased the hepatic venous portal gradient and preserved arterial flow to the graft [31]. Further research to clarify the efficacy of somatostatin infusion in LDLT recipients is necessary.
Although portal overflow might injure the graft directly, arterial vasoconstriction introduces secondary ischemic changes [32]. Our study showed that HAF increased after GIM, which was consistent with the hepatic artery buffer response [33]. However, we could not identify the optimal HAF or PVF-to-HAF ratio in our series.
A flowmeter (VeriQ™) is used to measure intraoperative flows. The system has been used in previous studies and produces reproducible measurements [34–36]. However, some limitations of this measurement were observed. First, flow rates are inevitably influenced by local and systemic factors (which are all subject to some degree of variance). Second, the instruments are sensitive to the proximity of the detector to the vessel and the manipulation required positioning of the probes.
Yagi et al reported a high-compliance (PVF/PVP) graft in which the PVF can be maintained at a high level, even though a low PVP was found to be a good graft for postoperative liver graft function [37]. Although intraoperative PVP data was incomplete in our study, we observed final PVP <15 mmHg in 89% of the patients in the modulation group.
This study had several limitations. First, this was a retrospective study with a small sample size at a single center. Second, the selection of the splenectomy over splenic artery ligation was an obligation, not an option. This might be considered a selection bias. Third, the recipients with collateral and splenorenal shunt ligation were excluded. The effect of low PVF was not studied. Finally, we did not follow a strict algorithm for GIM. In the future, we plan to develop and verify our algorithm.
Conclusions
In conclusion, we demonstrated that GIM was helpful for grafts with high PVF in adult LDLT to achieve satisfactory outcomes. Splenectomy modulated excessive PVF more effectively than SAL. Perioperative hepatic hemodynamic changes could assist surgeons in selecting strategies for GIM.
Tables
Table 1. Clinical characteristics of all recipients and donors.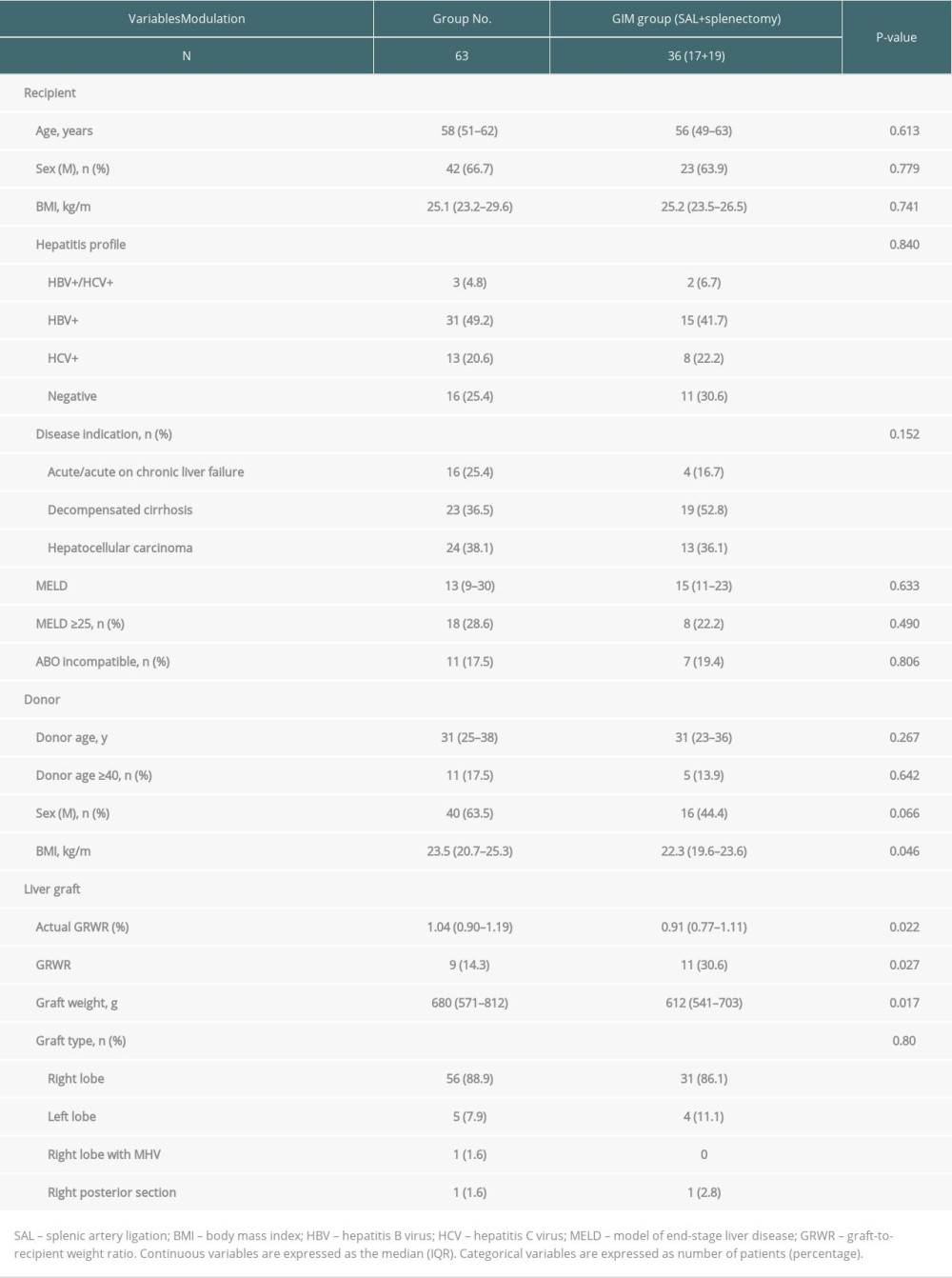 Table 2. Operative characteristics of all recipients and donors.
Table 2. Operative characteristics of all recipients and donors.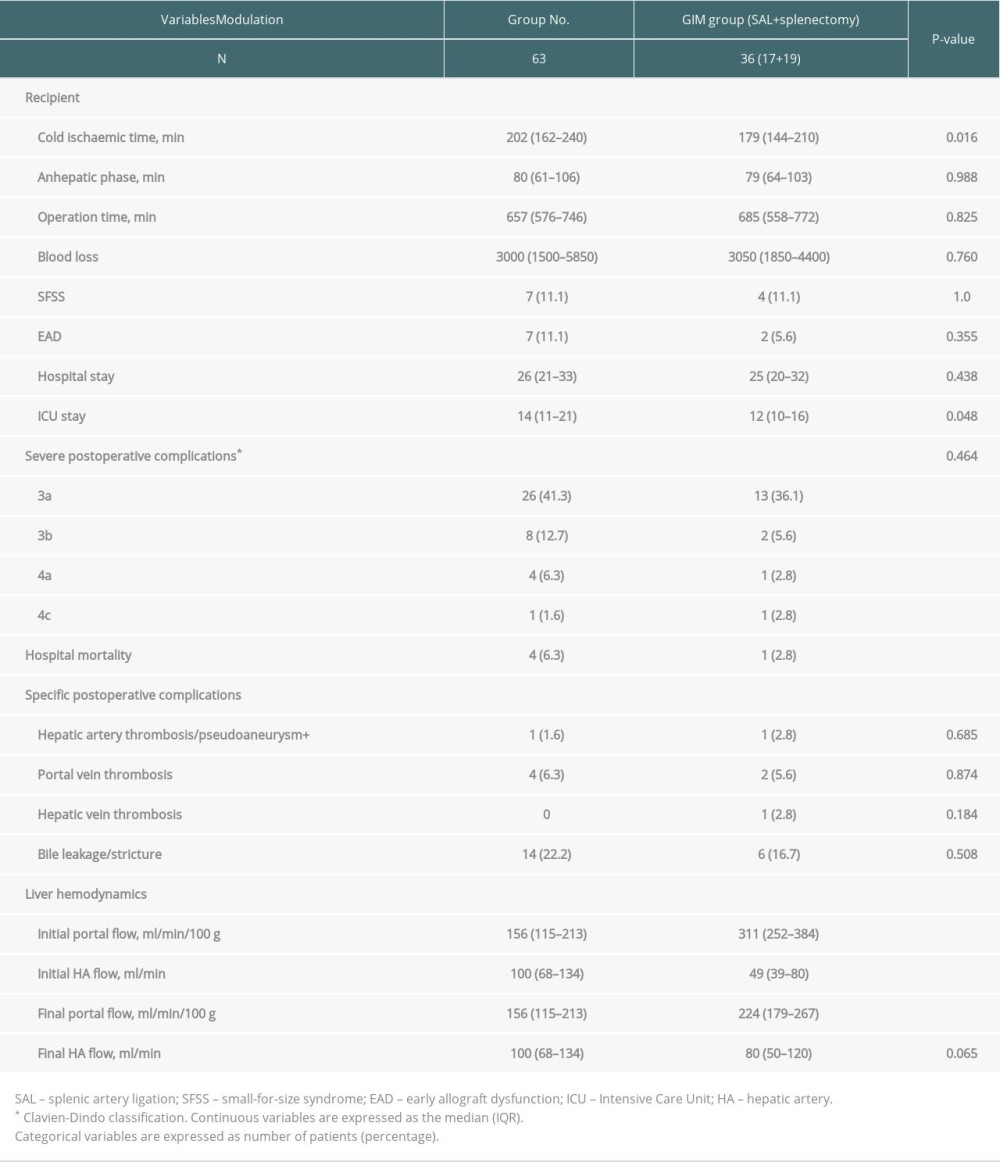 Table 3. Clinical characteristics of all recipients and donors in the modulation group.
Table 3. Clinical characteristics of all recipients and donors in the modulation group.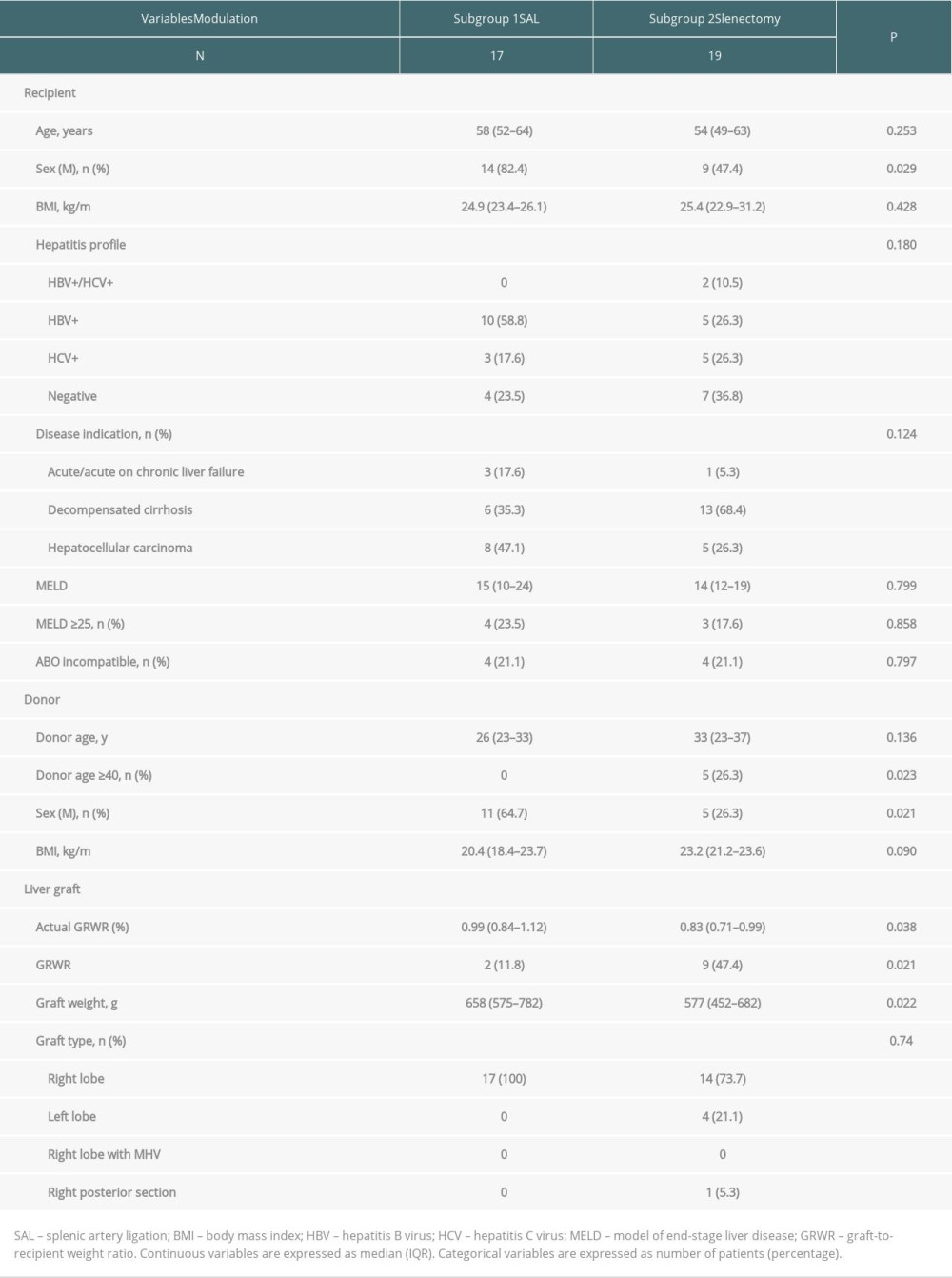 Table 4. Operative characteristics of all recipients and donors in the modulation group.
Table 4. Operative characteristics of all recipients and donors in the modulation group.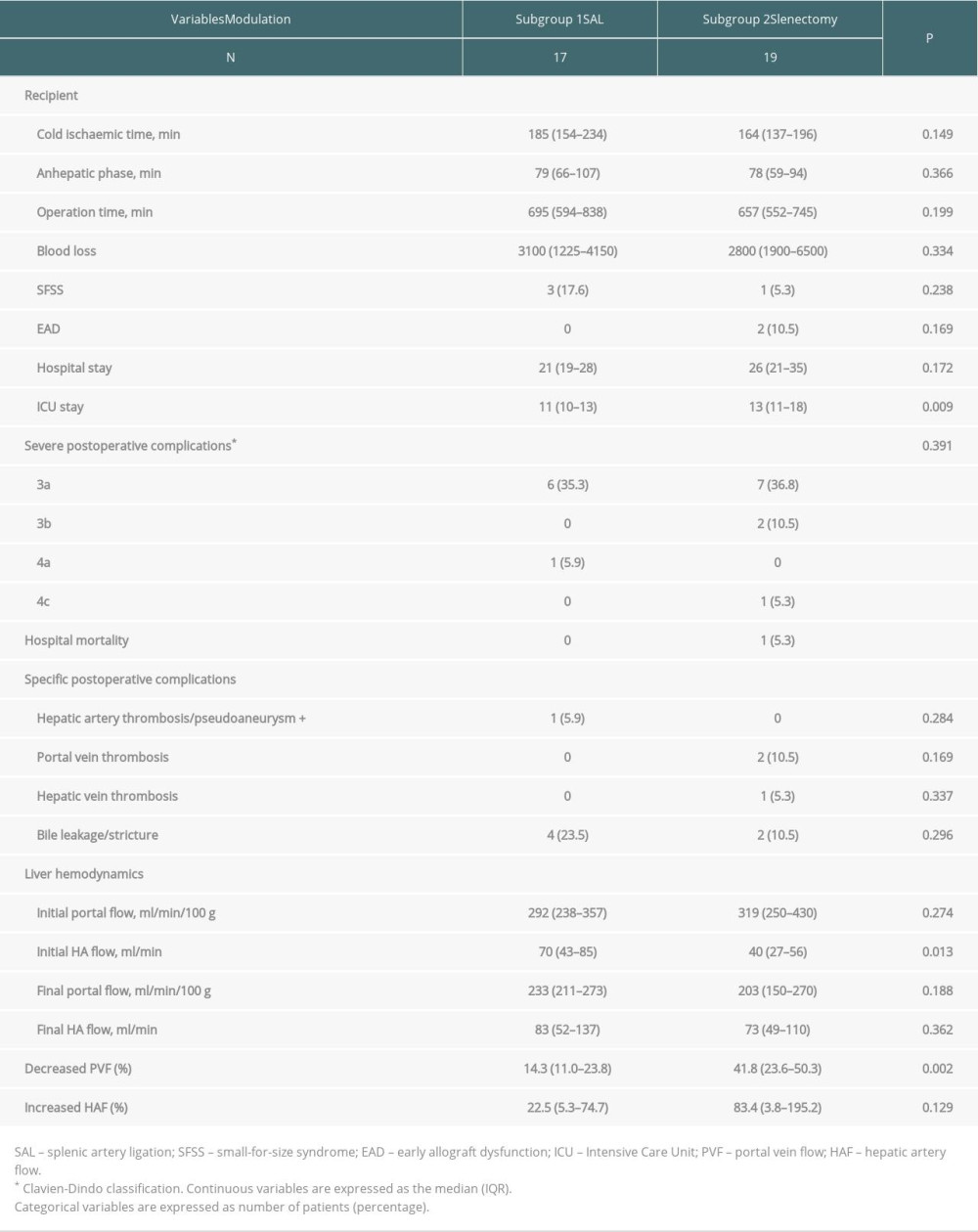
References
1. Inomata Y, Uemoto S, Asonuma K, Egawa H, Right lobe graft in living donor liver transplantation: Transplantation, 2000; 69(2); 258-64
2. Pomfret EA, Lodge JP, Villamil FG, Siegler M, Should we use living donor grafts for patients with hepatocellular carcinoma? Ethical considerations: Liver Transpl, 2011; 17(Suppl 2); S128-32
3. Dahm F, Georgiev P, Clavien PA, Small-for-size syndrome after partial liver transplantation: Definition, mechanisms of disease and clinical implications: Am J Transplant, 2005; 5(11); 2605-10
4. Kiuchi T, Kasahara M, Uryuhara K, Impact of graft size mismatching on graft prognosis in liver transplantation from living donors: Transplantation, 1999; 67(2); 321-27
5. Etesami K, Genyk Y, The increasingly limited basis for portal venous pressure modulation in living donor liver transplantation: Liver Transpl, 2018; 24(11); 1506-7
6. Ito T, Kiuchi T, Yamamoto H, Changes in portal venous pressure in the early phase after living donor liver transplantation: Pathogenesis and clinical implications: Transplantation, 2003; 75(8); 1313-17
7. Troisi R, Hoste E, Van Langenhove P, Modulation of liver graft hemodynamics by partial ablation of the splenic circuit: A way to increase hepatic artery flow?: Transplant Proc, 2001; 33(1–2); 1445-46
8. Ogura Y, Hori T, El Moghazy WM, Portal pressure <15 mm Hg is a key for successful adult living donor liver transplantation utilizing smaller grafts than before: Liver Transpl, 2010; 16(6); 718-28
9. Shimada M, Ijichi H, Yonemura Y, The impact of splenectomy or splenic artery ligation on the outcome of a living donor adult liver transplantation using a left lobe graft: Hepatogastroenterology, 2004; 51(57); 625-29
10. Yamada T, Tanaka K, Uryuhara K, Selective hemi-portocaval shunt based on portal vein pressure for small-for-size graft in adult living donor liver transplantation: Am J Transplant, 2008; 8(4); 847-53
11. Soin AS, Yadav SK, Saha SK, Is portal inflow modulation always necessary for successful utilization of small volume living donor liver grafts?: Liver Transpl, 2019; 25(12); 1811-21
12. Troisi R, de Hemptinne B, Clinical relevance of adapting portal vein flow in living donor liver transplantation in adult patients: Liver Transpl, 2003; 9(9); S36-41
13. Olthoff KM, Kulik L, Samstein B, Validation of a current definition of early allograft dysfunction in liver transplant recipients and analysis of risk factors: Liver Transpl, 2010; 16(8); 943-49
14. Sugawara Y, Makuuchi M, Takayama T, Small-for-size grafts in living-related liver transplantation: J Am Coll Surg, 2001; 192(4); 510-13
15. Fan ST, Lo CM, Liu CL, Safety and necessity of including the middle hepatic vein in the right lobe graft in adult-to-adult live donor liver transplantation: Ann Surg, 2003; 238(1); 137-48
16. Kaido T, Ogawa K, Fujimoto Y, Section 7. A new therapeutic strategy on portal flow modulation that increases donor safety with good recipient outcomes: Transplantation, 2014; 97(Suppl 8); S30-32
17. Sainz-Barriga M, Scudeller L, Costa MG, Lack of a correlation between portal vein flow and pressure: Toward a shared interpretation of hemodynamic stress governing inflow modulation in liver transplantation: Liver Transpl, 2011; 17(7); 836-48
18. Hayashi M, Fujii K, Kiuchi T, Effects of fatty infiltration of the graft on the outcome of living-related liver transplantation: Transplant Proc, 1999; 31(1–2); 403
19. Smyrniotis V, Kostopanagiotou G, Kondi A, Hemodynamic interaction between portal vein and hepatic artery flow in small-for-size split liver transplantation: Transpl Int, 2002; 15(7); 355-60
20. Lee S, Park K, Hwang S, Congestion of right liver graft in living donor liver transplantation: Transplantation, 2001; 71(6); 812-14
21. Soin AS, Smoothing the path: Reducing biliary complications, addressing small-for-size syndrome, and making other adaptations to decrease the risk for living donor liver transplant recipients: Liver Transpl, 2012; 18(Suppl 2); S20-24
22. Yagi S, Uemoto S, Small-for-size syndrome in living donor liver transplantation: Hepatobiliary Pancreat Dis Int, 2012; 11(6); 570-76
23. Emond JC, Goodrich NP, Pomposelli JJ, Hepatic hemodynamics and portal flow modulation: The A2ALL experience: Transplantation, 2017; 101(10); 2375-84
24. Lo CM, Liu CL, Fan ST, Portal hyperperfusion injury as the cause of primary nonfunction in a small-for-size liver graft-successful treatment with splenic artery ligation: Liver Transpl, 2003; 9(6); 626-28
25. Troisi R, Cammu G, Militerno G, Modulation of portal graft inflow: A necessity in adult living-donor liver transplantation?: Ann Surg, 2003; 237(3); 429-36
26. Yoshizumi T, Taketomi A, Soejima Y, The beneficial role of simultaneous splenectomy in living donor liver transplantation in patients with small-for-size graft: Transpl Int, 2008; 21(9); 833-42
27. Ito K, Akamatsu N, Ichida A, Splenectomy is not indicated in living donor liver transplantation: Liver Transpl, 2016; 22(11); 1526-35
28. Yoshizumi T, Itoh S, Shimokawa M, Simultaneous splenectomy improves outcomes after adult living donor liver transplantation: J Hepatol, 2021; 74(2); 372-79
29. Moon DB, Lee SG, Hwang S, Splenic devascularization can replace splenectomy during adult living donor liver transplantation – a historical cohort study: Transpl Int, 2019; 32(5); 535-45
30. Hessheimer AJ, Escobar B, Muñoz J, Somatostatin therapy protects porcine livers in small-for-size liver transplantation: Am J Transplant, 2014; 14(8); 1806-16
31. Troisi RI, Vanlander A, Giglio MC, Somatostatin as inflow modulator in liver-transplant recipients with severe portal hypertension: A randomized trial: Ann Surg, 2019; 269(6); 1025-33
32. Cantré D, Schuett H, Hildebrandt A, Nitric oxide reduces organ injury and enhances regeneration of reduced-size livers by increasing hepatic arterial flow: Br J Surg, 2008; 95(6); 785-92
33. Lautt WW, Mechanism and role of intrinsic regulation of hepatic arterial blood flow: Hepatic arterial buffer response: Am J Physiol, 1985; 249(5 Pt 1); G549-56
34. Abbasoglu O, Levy MF, Testa G, Does intraoperative hepatic artery flow predict arterial complications after liver transplantation?: Transplantation, 1998; 66(5); 598-601
35. Laustsen J, Pedersen EM, Terp K, Validation of a new transit time ultrasound flowmeter in man: Eur J Vasc Endovasc Surg, 1996; 12(1); 91-96
36. Lominchar PL, Orue-Echebarria MI, Martin L, Hepatic flow is an intraoperative predictor of early allograft dysfunction in whole-graft deceased donor liver transplantation: An observational cohort study: World J Hepatol, 2019; 11(9); 689-700
37. Yagi S, Iida T, Hori T, Optimal portal venous circulation for liver graft function after living-donor liver transplantation: Transplantation, 2006; 81(3); 373-78
Figures
Tables
 Table 1. Clinical characteristics of all recipients and donors.
Table 1. Clinical characteristics of all recipients and donors. Table 2. Operative characteristics of all recipients and donors.
Table 2. Operative characteristics of all recipients and donors. Table 3. Clinical characteristics of all recipients and donors in the modulation group.
Table 3. Clinical characteristics of all recipients and donors in the modulation group. Table 4. Operative characteristics of all recipients and donors in the modulation group.
Table 4. Operative characteristics of all recipients and donors in the modulation group. Table 1. Clinical characteristics of all recipients and donors.
Table 1. Clinical characteristics of all recipients and donors. Table 2. Operative characteristics of all recipients and donors.
Table 2. Operative characteristics of all recipients and donors. Table 3. Clinical characteristics of all recipients and donors in the modulation group.
Table 3. Clinical characteristics of all recipients and donors in the modulation group. Table 4. Operative characteristics of all recipients and donors in the modulation group.
Table 4. Operative characteristics of all recipients and donors in the modulation group. In Press
15 Mar 2024 : Review article
Approaches and Challenges in the Current Management of Cytomegalovirus in Transplant Recipients: Highlighti...Ann Transplant In Press; DOI: 10.12659/AOT.941185
18 Mar 2024 : Original article
Does Antibiotic Use Increase the Risk of Post-Transplantation Diabetes Mellitus? A Retrospective Study of R...Ann Transplant In Press; DOI: 10.12659/AOT.943282
20 Mar 2024 : Original article
Transplant Nephrectomy: A Comparative Study of Timing and Techniques in a Single InstitutionAnn Transplant In Press; DOI: 10.12659/AOT.942252
28 Mar 2024 : Original article
Association Between FEV₁ Decline Rate and Mortality in Long-Term Follow-Up of a 21-Patient Pilot Clinical T...Ann Transplant In Press; DOI: 10.12659/AOT.942823
Most Viewed Current Articles
05 Apr 2022 : Original article
Impact of Statins on Hepatocellular Carcinoma Recurrence After Living-Donor Liver TransplantationDOI :10.12659/AOT.935604
Ann Transplant 2022; 27:e935604
12 Jan 2022 : Original article
Risk Factors for Developing BK Virus-Associated Nephropathy: A Single-Center Retrospective Cohort Study of ...DOI :10.12659/AOT.934738
Ann Transplant 2022; 27:e934738
22 Nov 2022 : Original article
Long-Term Effects of Everolimus-Facilitated Tacrolimus Reduction in Living-Donor Liver Transplant Recipient...DOI :10.12659/AOT.937988
Ann Transplant 2022; 27:e937988
15 Mar 2022 : Case report
Combined Liver, Pancreas-Duodenum, and Kidney Transplantation for Patients with Hepatitis B Cirrhosis, Urem...DOI :10.12659/AOT.935860
Ann Transplant 2022; 27:e935860